The development of innovative microinvasive glaucoma surgery (MIGS) procedures has given us an opportunity to fill a long-existing niche in the glaucoma management. Traditionally, the treatment for mild to moderate glaucoma includes noninvasive and relatively safe topical medications and laser trabeculoplasty. MIGS offers new options for patients with mild to moderate open-angle glaucoma (OAG) who have failed medical or laser therapy but whose disease is not so advanced to warrant filtering surgeries, which pose a risk of vision-threatening complications from the surgery itself. This article offers a glimpse at the current and latest developments of MIGS.
MIGS procedures involve an ab interno, microincisional, conjunctivasparing approach with minimal tissue trauma and disruption of normal anatomy and physiology.1 The devices used for implantation exhibit a high level of biocompatibility. MIGS achieves moderate to high intraocular pressure (IOP) lowering efficacy, resulting in IOP in the mid-teens. The surgical techniques have a very good safety profile and allow for rapid recovery by the patient. All MIGS procedures are performed under gonioscopic view through a small side port incision. The ab interno techniques include removing trabecular meshwork tissue or implanting a shunt device.
Trabectome
Ab interno trabeculotomy by the Trabectome® device (NeoMedix, Tustin, USA) uses a high frequency electrocautery to remove a strip of trabecular meshwork and the inner wall of Schlemm’s canal (SC).2 The rationale for this angle surgery is the removal of the area of greatest resistance to aqueous outflow while achieving some retraction of the incision edges by heat effect and consequently reducing potential scarring. The device consists of a disposable hand piece, controlled via a 3-stage Foot Pedal Control that initiates irrigation, aspiration and electrocautery in sequence. No randomized controlled trials have been performed to date. Several studies have shown that the Trabectome alone and combined with phacoemulsification results in IOP levels ranging from 13.5 to 17.9 mmHg with greater reduction in patients with higher preoperative IOP and medication reduction from 21% to 38%.3–6 Jea and coworkers compared the safety and efficacy of the Trabectome to trabeculectomy with mitomycin C and concluded that the success rate of Trabectome was significantly lower. However, its excellent safety profile makes it a viable option for patients in which the risks of trabeculectomy are of particular concern, and patients in early disease stage, which typically involves more modest IOP goals.7
iStent
The iStent® trabecular micro-bypass stent (Glaukos, Laguna Hills, CA, USA) is a heparin-coated, non-ferromagnetic titanium device with a snorkel shape to facilitate implantation into SC and three retention arches in its outer surface to ensure secure placement. It is approximately 1×0.3 mm in size. It is placed using a single-use sterile inserter and directly connects the anterior chamber with SC. A systematic review and meta-analysis has shown that the iStent as a solo procedure without concurrent cataract surgery does lower IOP and reduces the dependency on glaucoma medications for up to 18 months post surgery.8 Although the data are limited, it suggests that the IOP decrease correlates with the number of iStents implanted. A 22% IOP reduction from baseline occurred at 18 months after one iStent implant, 30% at 6 months after implantations of two iStents, and 41% at 6 months after implantation of three iStents. The authors found a notable lack of published research on rates of early and late post-operative complications. The most common complications were related to iStent malposition or obstruction.
CyPass Micro-Stent
The CyPass® Micro-Stent (Transcend Medical Inc, Menlo Park, CA) is currently for investigational use in the United States. The rationale behind this polyimide, supraciliary device is to create a controlled cyclodialysis with stented outflow to the suprachoroidal space. This space is an attractive target due to its large surface area and negative pressure gradient, providing driving force for the aqueous outflow. The device is a 6.35 mm long tube with 300 μm lumen. It is inserted on a small guidewire with a special tip that separates the iris from the scleral spur allowing for the device to be inserted into the created cleft. Once the tube is in place, openings along its length allow aqueous to flow out. Hoeh et al. reported the one-year outcomes of the CyPass Clinical Experience (CyCLE) study.9 All subjects had OAG and underwent CyPass implantation during cataract surgery. Two analysis cohorts were pre-specified based upon medicated baseline IOP. Cohort 1 had initially uncontrolled IOP ≥ 21 mmHg, and 40 eyes had a 12-month follow-up visit. At that time, the mean IOP showed 35% decrease and there was a 49% reduction in medication usage. The second cohort had initially controlled IOP <21 mmHg. At the 12-month follow-up, 71 eyes were examined and found to have a 75% reduction in mean medication usage while maintaining mean IOP<21 mmHg. Fourteen percent of eyes had transient early hypotony, which resolved by 1 month in all cases, without requiring any surgical intervention. A multicenter, singlearm interventional study, using CyPass alone, showed a 35% reduction in IOP and a 36% reduction in medication use at 1-year follow-up (n=65).10 Eighty three percent of eyes avoided conventional filtering surgery.
Schlemm’s Canal Scaffold
The Hydrus™ Microstent (Ivantis, Inc., Irvine, CA, USA) is an 8 mm long device made of highly elastic biocompatible material called nitinol. It is a crescent-shaped open structure, curved to match the shape of the SC. The idea of this “intracanalicular scaffold” is to maintain SC’s patency over 3 clock hours upon insertion and provide direct aqueous access from the anterior chamber to multiple collector channels. It is currently for investigational use in the United States. The Hydrus II study included 100 patients (50 per treatment arm), who were randomized to have phacoemulsification with Hydrus or phacoemulsification alone.11 All patients underwent medication washout prior surgery with baseline diurnal IOP of about 26 mmHg in both arms. At 2-year follow-up the washed-out mean diurnal IOP in the Hydrus plus phacoemulsification group was significantly lower compared with the phacoemulsification alone group, at 16.9±3.3 mmHg versus 19.2±4.7 mmHg (50% versus 28% reduction), respectively. The proportion of patients using no hypotensive medications was significantly higher at 24 months in the Hydrus plus phacoemulcification group (73% versus 38%).
Subconjunctival Implant
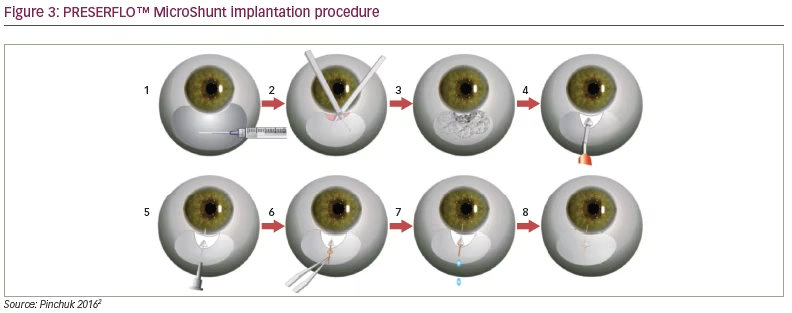
The XEN® Gel Stent (AqueSys Implant) was created by AqueSys Inc (Aliso Viejo, CA, USA). It is made out of a soft collagen-derived gelatin that is known to be non-inflammatory. The goal of the implantation is to create an aqueous humor outflow pathway from the anterior chamber to the subconjunctival space. The implant is 6 mm long and about the width of a human hair, preloaded in a needle tip injector. Similar to the other implants, it can be performed in conjunction with cataract surgery. It is an investigational device currently undergoing clinical trials.
MIGS technology opens an exciting new chapter in the current glaucoma management. It has the potential to address numerous challenges we face in our daily glaucoma practice, e.g., patient adherence, ocular toxicity, cost of glaucoma medications, etc. MIGS ab interno approach avoids conjunctival manipulation, preserving the more invasive surgery options. Future randomized control studies will hopefully provide us with knowledge about long-term efficacy, ideal patient selection, optimal location for device implantation, and cost-effectiveness data.