The successful management of glaucoma is still a challenge, especially in low-resource countries, where treatment options are limited. Awareness about glaucoma is often low in the general population and even amongst patients with glaucoma themselves.1–3 More than 50% of patients present to the clinic when the disease has reached an advanced stage.4–6 The goal of glaucoma treatment is to retain the patient’s vision-related quality of life by reducing the damaging intraocular pressure (IOP) to a level where further glaucomatous damage of the retinal ganglion cells ceases.7,8 The reduction of IOP is currently the only modifiable risk factor in glaucoma treatment.9,10 IOP reduction is achieved with medical treatment, laser treatment, surgery or a combination of these options.
Generally, medical therapy is most often the choice of treatment for glaucoma, although laser treatment is now being promoted and offered as a first-line treatment option.11–14 Surgery is usually recommended when the IOP is uncontrollable despite maximally tolerated medical therapy, if there is intolerance or non-adherence to medical therapy, as a first-line treatment in advanced stage, juvenile and congenital glaucoma or if there is poor adherence to medical therapy or poor access to care.15–17 Surgery is the most cost-effective treatment option in advanced glaucoma and is the recommended method of treatment in low-resource economies.15,18–20 As a result, glaucoma surgery is expected to be common in Sub-Saharan Africa, where most countries are resource constrained and most patients present with advanced disease. However, many authors have found practice of glaucoma surgery among ophthalmologists to be low in the country.21–23 The most frequently reported reason for the low number of glaucoma surgeries in Africa has been poor acceptance of surgery by patients,17,24–26 with an acceptance rate of between 6 and 46%.22,25,27 Major reasons for refusal found by authors include no visual improvement from surgery, cost and fear of surgery/blindness.24,25 Some authors have also reported that there is poor awareness of glaucoma treatment options outside of medical therapy.28,29 In the event of medical treatment failure, it is presumed that prior knowledge of the various alternative treatment options available might prime a patient for the acceptance of a second-line option.
The last study in Nigeria on this subject was reported about 7 years ago, and there has been an increased (though uncoordinated) effort at educating patients and the public with glaucoma during the intervening period.29 The current level of awareness of glaucoma surgery is not known. This study, therefore, sought to determine the awareness level of incisional surgical treatment as an option for patients with glaucoma receiving medical treatment and to identify the reasons for non-uptake when surgery was recommended.
Materials and methods
From January 2016 to December 2018, a two-centre cross-sectional survey was carried out on consenting patients with primary (open-angle [POAG] and closed-angle [PACG]) glaucoma already taking medical treatment. The patients attended glaucoma clinics at The Eye Specialists Hospital (TESH, a private eyecare facility) and ESUT Teaching Hospital Parklane (ESUTTHP, a public health facility), both in Enugu, Nigeria.
All participants were ≥40 years, on glaucoma medical treatment and with a vertical cup-disc ratio of ≥0.8. These patients are more likely to be candidates for surgery. Patients with ocular hypertension, early/pre-perimetric glaucoma, glaucoma suspects, secondary glaucoma, post-glaucoma surgery/laser patients and those who did not give their consent were excluded from the study.
In the glaucoma clinics, pre-tested questionnaires were administered to consenting, eligible patients by trained research assistants. The questionnaire was designed by the authors to provide relevant answers to the study questions. It was presented to a statistician, who established construct validity. The questionnaire was then reviewed for content validity by an external senior ophthalmologist who specializes in glaucoma. It took an average of 7 minutes to administer the questionnaire to each participant. The questions sought to ascertain the participants’ socio-demographics, awareness of surgery as a glaucoma treatment option and willingness to take up surgery if recommended.
Only the patients who were aware of and had been offered glaucoma surgery were asked for their reasons for non-uptake. Open-ended questions were used to ascertain their reasons.
Participants underwent ocular examinations, including visual acuity measurements using Snellen’s chart, vertical cup-disc assessments using slit lamp biomicroscopy (with +78D/+90D condensing lens) and visual field analysis using an OCULUS Twinfield® machine (OCULUS Optikgeräte GmbH, Wetzlar, Germany). To have comparable result, one visual field machine positioned in TESH (the private facility) was used for both centres. Some of the patients who could not move from ESUTTHP to TESH did not do the visual field test. Blind participants and those with severe visual impairments, who could not see the target on the visual field test, were recorded under advanced field loss. Where the level of visual loss was same in both eyes, they were recorded under ‘better eye’ and ‘worse eye’ separately.
For ease of computing and analysis, the findings were grouped based on the level of severity.
Results from the visual acuity measurements were grouped according to the World Health Organization classification: mild (visual acuity worse than 6/12–6/18), moderate (visual acuity worse than 6/18–6/60), severe (visual acuity worse than 6/60–3/60), blindness (visual acuity worse than 3/60).30
Results from the central visual field measurements were categorized according to the Anderson criteria: early defect (mean deviation [MD] of less than -6dB), moderate defect (MD of less than -12dB), severe defect (MD of greater than -12dB).31,32
For ease of the logistic regression analysis, the social and clinical characteristics of the patients were further re-grouped according to age, education, visual acuity, duration of glaucoma and visual field damage.
Data were analyzed using IBM® Statistical Package for Social Sciences (SPSS)® version 22. Means and standard deviations were calculated for the quantitative variables, while frequencies and percentages were calculated for the qualitative variables. Frequency tables were generated for the variables. Logistic regression analysis was used to identify possible predictors of awareness of glaucoma. P-value of <0.05 was statistically significant.
Ethical approval was obtained from the Ethical Review Committee of ESUTTHP, Enugu, Nigeria. Written informed consent was obtained from all patients taking part in the study. The study abided by the guidelines of the 2013 Declaration of Helsinki for studies involving human subjects. Confidentiality was assured and ensured, and participants were free to withdraw at any phase of the study free of any consequences.
Results
A total of 299 patients with glaucoma participated in the study: 167 participants were male (55.9%), and 132 were female (44.1%). The mean age was 63.9 ± 11.9 years (range 40–103 years). Two hundred and sixty-seven participants (89.3%) had received a formal education (defined as a structured or systematic form of learning that usually runs from primary to post-university education). The duration of disease diagnosis among participants ranged from 1 to 360 months. Sixty-two participants (20.8 %) were diagnosed with glaucoma ≤12 months before the study began, 146 participants (48.8%) were diagnosed within 13–60 months of the study beginning, and 91 participants (30.4%) were diagnosed >60 months prior to the study beginning (Table 1).
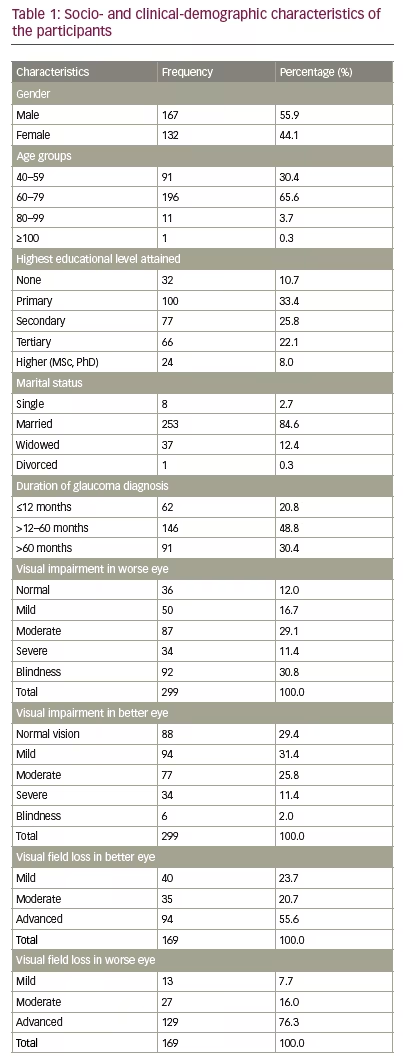
In the better eye of the 299 participants, 88 (29.4%) had normal vision, 171 (57.2%) had mild-to-moderate visual impairment, 34 (11.4%) had severe visual impairment, and 6 (2.0%) were bilaterally blind. In the worse eyes of the 299 participants, 36 (12.0%) had normal vision, 137 (45.8%) had mild-to-moderate visual impairments, 34 (11.4%) had severe visual impairments, and 92 (30.8%) were blind (Table 1).
Of the 169 participants (out of 299) whose visual field analysis was performed on at least one eye, 23.7%, 20.7% and 55.6% had mild, moderate and advanced glaucoma in the better eye, respectively. In the worse eye, 7.7%, 16.0% and 76.3% had mild, moderate and advanced glaucoma, respectively (Table 1). In all the eyes, the vertical cup-disc ratio was ≥0.8.
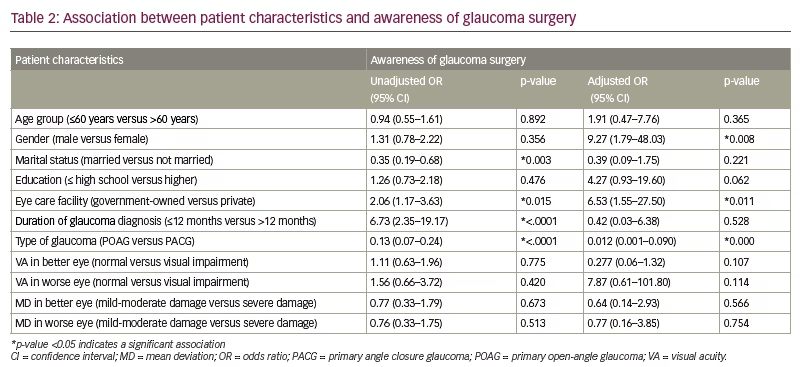
Among the 299 participants, 79 (26.4%) were aware of surgery as a treatment option for glaucoma, while 220 (73.6%) were unaware. Using univariate analysis, we found that factors significantly associated with awareness of surgery were marital status, duration of glaucoma diagnosis, type of eye care facility and type of glaucoma. The odds ratio (OR) of awareness was calculated for married versus not currently married (OR 0.35; 95% confidence interval [CI] 0.19–0.68), duration of glaucoma diagnosis of ≤12 months versus >12 months (OR 6.73; 95% CI 2.35–19.17); government-owned eyecare facility versus private facility (OR 2.06; 95% CI 1.17–3.63) and type of glaucoma (POAG versus PACG; OR 0.13; 95% CI 0.07–0.24). By multivariate analysis, we found that gender, type of eye care facility and type of glaucoma were significantly associated with awareness (Table 2).
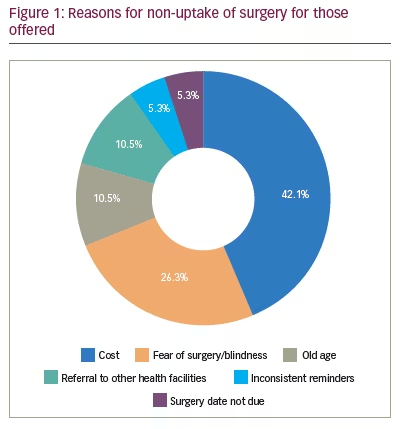
Of the 79 participants who were aware of the surgical treatment option for glaucoma, 19 (24.1%) had been offered surgery by their ophthalmologists. Patients were offered surgery because their glaucoma progressed despite the use of maximum doses and the combination of glaucoma medications, which resulted in persistently high IOP and progressive loss of visual field. Among these 19, none had undergone surgery. Eight (42.1%) had not undergone surgery due to cost, and five had not had surgery (26.3%) due to fear of blindness or the surgery itself, while the rest had not yet had surgery because of old age or had been referred to another health facility to have the surgery (Figure 1).
Discussion
According to the American Medical Association Journal of Ethics, patients are free to exercise their autonomy in making decisions about their health care, provided they are given information about and understand the risks and benefits of a specific treatment.33 It has also been noted that giving patients choices is important and has been linked to patient satisfaction, although it may provide challenges in healthcare.34
There is a great assumption that patients with glaucoma are aware of the different treatment options available, despite the existence of relatively few publications available on the subject, especially in developing countries. However, only 26.4% of patients with primary glaucoma on medical treatment in this study were aware of the surgical treatment option. Results from this study population show that, despite the patients’ level of education, age degree of visual impairment and visual field loss, they were grossly unaware of the surgical treatment option for glaucoma. Conversely, a previous study (in Nigeria) by Nwosu found that 61.5% of patients with glaucoma who were already on medication were aware of both medical and surgical treatment options.29 This difference could be from differences in study age groups and study size, as well as the latter being a one centre study. Nwosu’s study the age group as low as 16years and a total study size of 52 as against 40years and 299 respectively in this study.29 Other studies conducted in developed economies such as Germany and Switzerland also found awareness of surgery as a treatment option of 63% and 75%, respectively.35,36 However, other studies in the general population have found an awareness of surgery as a treatment option of 14% in Nigeria and 3.5% in India.2,37 The high-level lack of awareness in these studies may be a reflection of the content and effectiveness of the eye health education/counselling available to patients with glaucoma in these countries.
The increased lack of awareness of the surgical treatment option among our study population (73.6%) suggests insufficient or deficient glaucoma information, education and counselling services. It is also presumable that, because the practice of glaucoma surgery (trabeculectomy) among ophthalmologists in the study country is low, patients are often not informed of the surgical option by their ophthalmologists.21,23 This is notable, as 76.3% of patients had advanced glaucoma in their worse eye based on visual field grading, yet only 79 patients had heard of the surgical treatment option and only 19 patients indicated that surgery had been recommended for them.21,23 This further highlights the need for good glaucoma surgical training during postgraduate training, as the practice of trabeculectomy has been strongly linked to the degree of exposure during the residency programme.23
Multivariate analysis identified that patients with PACG were more likely to be aware of the surgical option than POAG. PACG is generally more likely to require a surgical procedure than POAG.38,39 This may explain why patients with PACG in this study were more aware of surgery than those with POAG.
Study participants who received care from the private facility were also found to be more likely to be aware of surgery than those from the government-owned facility. Adekoya et al. also reported higher uptake of glaucoma surgery in privately owned eye care facilities compared with government-owned facilities, even when the clinic burden in the private centres was the lowest.21 Lower burden of patients in private centres probably affords eye care providers more time to discuss with and educate patients on the different glaucoma treatment options available. The other main identifiable difference between the two facilities in this study was the presence of a counselling unit in the private eye facility. However, the counselling unit was only partially functional. Patient counselling has been found to improve patients’ knowledge and awareness of their ailment and to improve acceptance of glaucoma surgery.40–42 Incorporating routine counselling into glaucoma care service protocols will likely ensure the standardization of information reaching the patient.
In this study, gender was found to be associated with awareness of glaucoma. Although, in general, women are considered less empowered financially than men, they are often more likely to seek healthcare when needed. In this study population, more women were empowered financially, hence may not be as dependent on men to access healthcare. In addition, due to childbirth and childcare, women are more likely to visit health facilities more often. This may result in more exposure to information from healthcare providers, which is likely to increase the health awareness of women. In contrast, men are unlikely to seek care if hospital visits or prescribed treatments are likely to impact their livelihood.
Glaucoma in Africa is more aggressive, responds poorly to treatment and leads to blindness faster than in other areas of the world.4,24 Therefore, surgery should potentially be offered more frequently when there is poor IOP and disease control. However, even when offered, patients do not always agree to surgery, as there may be other barriers. Out of the 19 participants who were offered surgery, the cost involved was the most common (42.1%) barrier to uptake. Although glaucoma surgery is a cost-effective method of treatment, the initial high cost of surgery in the face of limited health insurance schemes can be challenging.17,43 Achigbu et al. found that, out of 54 patients, only 14 (25.9%) considered surgery as a way to reduce the cost of management.44 Therefore, improving the understanding of the cost-effectiveness of surgery may improve the willingness to undergo surgery.
At this time, the majority of evidence available suggests that surgery reduces IOP more significantly than medical therapy, although a few studies have found similar efficacies between medical and surgery therapies.5,45–47
The World Glaucoma Association recommends glaucoma surgery as a primary treatment in resource-constrained economies.20,43,48 However, the acceptance rate of surgery among patients with glaucoma in Africa has been found to be between 6.7 and 46.0%; notably, the rate is higher among patients newly diagnosed with glaucoma (32.5–68.6%).24,25,27,29,49 If patients in these areas are better informed of the cost-effectiveness of glaucoma surgery through counselling, this could lead to a greater acceptance of surgery.
Fear of surgery and blindness were the second most common barrier (26.3%) to surgery. Olatunji et al. reported that previous poor surgical outcomes in patients’ acquaintances accounted for 31% of the reasons for refusing surgeries.50 The fear of vision loss has also been identified as a major cause of refusal among general eye patients.51,52 Trabeculectomy has a technical success rate of approximately 65–80%.17,20,53 Previous studies identified other reasons for declining surgery to include worries about a lack of vision improvement after surgery, surgical complications, fear of blindness, fear of surgery and negative publicity.24,25,54 This reinforces the need for good surgical outcomes and well-informed patient consent. Better surgical skills lead to better outcomes.21,23
In countries with high life expectancy, the prevalence of POAG is associated with older age and is 3.9–6.5%, 1.95–3.2% and 2.1–3.0% in Japan, Singapore and Australia, respectively.55-60 The prevalence of glaucoma in these regions is generally low compared with what we have in the developing world. Although Japan has a glaucoma prevalence higher than that of some countries in Africa, rates of blindness due to glaucoma in Japan are far below those in Africa. In Nigeria, the prevalence of glaucoma is 5.02%, with 20% of patients with glaucoma suffering from blindness, whereas in Singapore, the glaucoma prevalence is 3%, with blindness affecting 0.05% of patients.61
Although glaucoma may be a major cause of blindness in countries with a high life expectancy, most of those countries enable access to high-quality healthcare, which ensures that the healthcare needs of older people are addressed. This may bring about early diagnosis and access to treatment, which may delay the onset of blindness and lead to a low prevalence of blindness. In developing countries, however, access to healthcare services and availability of treatment are below optimum. Even when available, cost poses a challenge to uptake. This may mean that, even though life expectancy is reduced, those who already have glaucoma may not have access to the treatment, increasing the burden of blindness in these areas.
Strengths and limitations
This study sampled participants from government-owned and private eye care facilities: therefore, participants were from varied socio-economic backgrounds. The study determined patients’ awareness of surgery as a treatment option for glaucoma and also determined reasons for non-uptake of surgery when offered.
This study has some limitations. Central visual field analysis was not carried out on some participants for various reasons. This led to incomplete data required for full comparisons and analysis. The number of participants included in the analysis of barriers to surgery uptake was small.
Conclusions
Awareness of surgery as a treatment option for glaucoma was low among patients with primary glaucoma receiving medical treatment. Cost and fear of blindness were the main barriers to the uptake of surgery. Incorporating glaucoma surgery into counselling and education, including as a treatment option, into glaucoma care protocols will likely improve awareness of surgery as a treatment option.







