The tear film is fundamental in the maintenance of the ocular surface: alterations in quantity or quality result in an unstable tear film and onset of an ocular surface disease and/or a dry eye syndrome. The 2007 report of the International Dry Eye Workshop (DEWS) classified dry eye as caused by decreased tear secretion or by increased evaporation (by intrinsic or extrinsic causes).1
The tear film is fundamental in the maintenance of the ocular surface: alterations in quantity or quality result in an unstable tear film and onset of an ocular surface disease and/or a dry eye syndrome. The 2007 report of the International Dry Eye Workshop (DEWS) classified dry eye as caused by decreased tear secretion or by increased evaporation (by intrinsic or extrinsic causes).1
Glaucoma is a chronic neuropathy in which the topical medications usually represent the standard of therapy:2 the pressure-lowering eyedrops are generally preserved and may induce ocular surface disorders attributable both to the drugs themselves and to the drugs preservatives. In fact, the prolonged use of preserved topical drugs is an extrinsic cause of increased tear evaporation, which induces a toxic response from the ocular surface. Benzalkonium chloride (BAK) is the most commonly used preservative in ophthalmic solutions, especially in anti-glaucoma drugs; it has a well-known dose-dependent toxicity.3,4 Its cellular toxicity has been experimentally demonstrated in in vitro studies of conjunctiva-derived and corneal cells.5,6 BAK excites the expression of inflammatory cell markers at the ocular surface,7 causes epithelial cell damage, cell death by apoptosis and a decrease in goblet cell density leading to tear film instability and tear hyperosmolarity.8–10 The subsequent surface epithelial cell damage and punctate epithelial keratitis interfere with surface wettability.1
Dry eye represents a common disorder in the elderly11,12 but is usually insufficient to cause any severe symptoms. Age-related dry eye has been widely studied: Mahlers et al., in 1996, reported that changes in lachrymal evaporation, volume and osmolarity of the tear film is significantly associated with normal ageing;13 Craig and Tomlinson,14 Sahlin15 and Rolando,4 did not point out any significant relation. In glaucoma patients over 40 years old, BAK-linked effects usually combine with age-related dry eye.12
The impact of dry eye on a glaucoma patient’s daily life, particularly symptoms of discomfort, is an important aspect to consider in the follow-up. In a recent study of 61 glaucoma patients topically treated, we pointed out that all patients with an ocular surface disease recorded lower quality-of-life scores versus patients without surface changes.16
Authors will suggest a sequence of ophthalmic examinations that should be performed to glaucoma patients to point out ocular surface alterations in clinical practice.
It must be remembered that a poor correlation has been found between objective and subjective signs of dry eye disease,17–19 underlining that a patient’s self-assessment of dry eye severity may differently relate to objective signs.
Sequence of Tests
The diagnosis of ocular surface disease is based both on symptoms reported by the patients (history and ‘dry eye questionnaires’) and on signs recorded by the ophthalmologist (objective tests).
Symptoms Tests
Symptoms reported by glaucoma patients can be collected and have been used to diagnose the condition in several previous studies, but the use of a questionnaire to assess the symptoms and their impact on vision-related function is preferable, since the answers are standardised and comparable over time.
A number of instruments have been developed to understand patients’ experience of ocular surface disease and its impact on their quality of life. Some studies developed ways of measuring patient-reported symptoms of dry eye, such as the Shein questionnaire,19 the McCarthy symptom questionnaire,20 the Dry Eye Questionnaire,21 the McMonnies questionnaire,22 the Impact of Dry Eye on Daily Life (IDEEL) questionnaire23 and the Ocular Surface Disease Index (OSDI).24 A few glaucoma patient-specific questionnaires have been developed, such as the Treatment Satisfaction Survey for Intraocular Pressure (TSS-IOP)25 and the Glaucoma Symptom Scale (GSS).26
To be routinely adopted into clinical practice, a questionnaire must be easy and fast to complete; for these reasons we suggest using OSDI and/or GSS.
The OSDI is a disease-specific questionnaire used to quantify the specific impact of dry eye on vision related quality of life (see Figure 1). It includes three subscales: ocular discomfort (OSDI-symptoms), functioning (OSDI-function) and environmental triggers (OSDI-triggers).24 The questions refer to a one-week recall period and possible responses refer to the frequency of the disturbance. OSDI subscale scores can range from zero to 100, with higher scores indicating more problems or symptoms. The OSDI score is calculated as: (sum of scores x 25) ÷ (the total number of questions answered). The OSDI evaluates the impact of dry eye with the following scores: 0–12 (normal), 13–22 (mild), 23–32 (moderate) and 33–100 (severe). This questionnaire has been reported to have excellent test-retest reliability and to effectively discriminate between normal, mild-to-moderate and severe ocular surface disease.24
The GSS26 is a disease-specific questionnaire used to quantify the specific impact of glaucoma either on visual ocular complaints or non-visual ocular symptoms (see Figure 2). The questions refer to a four-week recall period. For each eye, a five-level score ranging from zero to 100 was generated, with zero representing the presence of a very bothersome problem and 100 representing the absence of a problem. It includes a function subscale, a symptoms subscale and an overall average score. All subscales may be evaluated as the average of both eyes or separately for each eye. The GSS has been shown to discriminate between persons with and without glaucoma.
Signs
Dry eye syndrome is diagnosed by objective methods that examine different aspects: tear flow (Shirmer I and II, evaporimetry, fluorimetry, dye dilution, etc.); tear stability (break-up time [BUT]), symptomatic BUT (SBUT), fluorescein tear film break-up time (TF-BUT), non-invasive BUT (NIBUT), tear stability analysis system, etc.; tear composition (lactoferrin, lysozyme, peroxidase, immunoglobulin A, impression cytology, flow cytometry, confocal microscopy, interferometry, osmolarity, tear ferning, grading staining, fluorescein stain, rose bengal stain, lissamine green, etc.)1,27,28
The following examinations (the Shirmer’s test, TF-BUT and the corneal staining [fluorescein and/or lissamine]) can be easily performed by the ophthalmologist in daily practice.
The Shirmer’s test I (without anaesthesia) is an indicator of the reflex tear flow. Patients are asked to look up and the lower eyelid is drawn gently downwards and temporally. The rounded bent end of the sterile strip is hooked in the lower cul-de-sac over the junction of the temporal and central one-third of the lower eyelid margin. The testing period is initiated. To minimise the potential for conjunctival staining from this test, the patients are asked to gently close their eyelids until five minutes had elapsed and the strips are removed. The amount of wetting is measured using the graduated paper scale included in the box of strips. The Schirmer test is normal if >10 mm and abnormal otherwise (mild to moderate between six and 10mm; and severe, zero to 5mm).
Tear film stability can be assessed using the TF-BUT method. A wet fluorescein-impregnated strip is placed in the inferior fornix or a drop of 2% sterile fluorescein is instilled into each conjunctival sac with a micro-pipette and the patient is asked to blink several times. The TF-BUT is evaluated measuring the interval between a complete blink and the appearance of the first area of tear film break-up on the corneal tear film, using a cobalt blue filter on the slit lamp microscope. The TF-BUT values greater than or equal to 10 seconds are coded as normal and TF-BUT values less than 10 seconds as abnormal.29,30 The TF-BUT is usually performed prior to grading.
Corneal staining can be determined with different dyes: with fluorescein, staining must be graded as quickly as possible after instillation, since the dye then diffuses rapidly into the tissue and its high luminosity blurs the stain margin; staining after lissamine green, persists at high contrast and may therefore be observed for a considerable period.
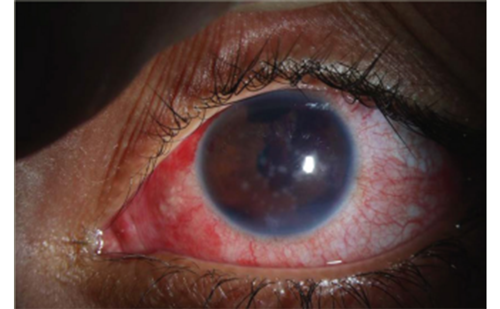
The presence of corneal staining can be defined as more than one dot of fluorescein staining over the corneal surface. Since fluorescein diffuses rapidly into tissues, it is to assess staining rapidly, in sequence, in the right and then the left eye, so that the staining patterns observed are equally crisp. Superficial punctate keratitis can be graded according to the corneal fluorescein staining scale by determining the area and density of the lesion on a zero to three scale, where zero indicates the absence of keratitis punctata, one equals mild (a few punctata of staining but less than 10% coverage of the corneal surface; two equals moderate (10–50% coverage of the corneal surface); and three equals severe (more than 50% coverage of the corneal surface [see Figure 3]).31
Lissamine green is available as impregnated strips or may be ordered as a pre-prepared solution. A 1% drop will give more intense staining. Because the drop is well tolerated, no anaesthetic is required. Using white light of moderate intensity, staining at the corneal region and the interpalpebral region of the nasal and temporal conjunctiva is graded using the Oxford Scheme.31 The severity designations used for lissamine green staining are the following: 0 to I is normal; II to III is mild to moderate; and IV to V is severe (see Figure 4). Since this dye does not diffuse into the substantia propria of the conjunctiva, the staining pattern is retained for longer.
Discussion
Glaucoma is a chronic disease that is often treated with topical drugs. Unfortunately, the chronic use of most IOP-lowering medication is associated with some symptoms of toxicity, such as ocular inflammation, allergy and dry eye. This toxicity has been associated with the preservative BAK, which damages conjunctival and corneal epithelial cells. A recent paper on a rabbit dry eye model induced by topical BAK10 demonstrated that BAK causes damage to the cornea and conjunctiva, decreases tear basal secretion and globlet cell loss and MUC5AC deficiency. Recent studies32–35 pointed out that the exclusive use of preservative-free eye drops clearly reduces the signs of ocular surface alteration in glaucoma patients and that the use of alternatively preserved glaucoma medications cause minimal adverse effects on the ocular surface compared with drugs with high BAK levels. Despite this, to date, the majority of glaucoma medications are still preserved.
Thygesen et al. in 2000,36 Costagliola et al. in 200137 and Rossi et al. in 2009,16 evaluating prostaglandin analogues in the ocular surface, concluded that prostaglandin analogues were safer on ocular surface function than topical timolol. Pisella and Badouin in 2004,8 compared in the same conjunctival cell line the pro-apoptotic effects of timolol and latanoprost when associated with the same 0.02% BAK concentration: the decrease in apoptosis and cell viability levels observed with prostaglandin analogue were significantly lower than those induced by preserved timolol.8 Prostaglandin derivatives may have a relative protective effect against the toxicity of this preservative on conjunctival cells. Okada’s paper on the effects of topical medication evaluated by gene expression patterns6 disagrees with these conclusions: the mechanism remains to be determined and further investigation on humans are required. Moreover, age13,14 and diabetes1,38–40 represent risk factors involved in the development of ocular surface disease: glaucoma patients are therefore, presumably at a higher risk for developing ocular surface disease as both diseases are more common in older and in diabetic patients.
Usually, glaucoma patients undergo several specific and complex tests to evaluate morphology (hormone replacement therapy [HRT], optical coherence tomography [OCT], GDxTM Nerve Fiber Analyzer [GDx]) and function (visual field [VF], pattern electroretinogram [PERG]). Recent literature suggests the impact that an abnormal ocular surface status could have on patients’ wellbeing.16,41 The ocular surface status should be evaluated regularly before starting a new chronic topical therapy and during the follow-up to ensure the timely detection and treatment of pathological signs on the ocular surface. A misdiagnosed and consequently, untreated dry eye may alter vision. These negative effects should be added to glaucoma’s natural evolution and progression.
In conclusion, a complete ocular examination comprehensive of the ocular surface evaluation should be performed on each glaucoma patient before starting a topical therapy and in the follow-up. The tests suggested in this article to verify the presence of ocular surface alteration are simple, easy to perform and require little time. ■