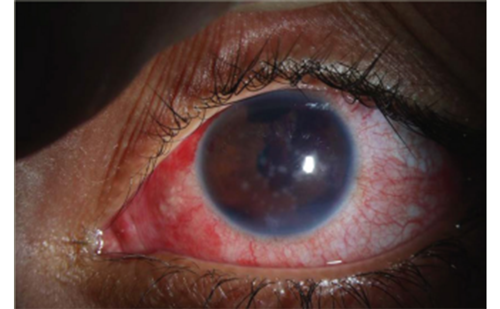
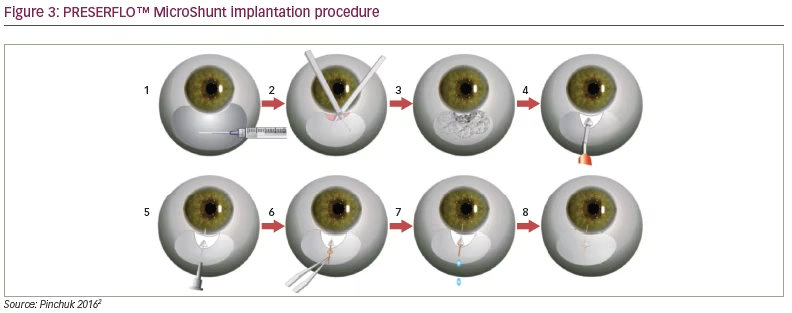
Primary open-angle glaucoma (POAG) is a chronic and usually bilateral disease. It can vary in time and onset and is characterised by abnormalities in the visual field that are caused by loss of optic nerve fibres. Open anterior chamber angle is characteristic in this disease. Typical form of secondary open-angle glaucoma is pseudoexfoliative glaucoma (XFG).1 Here, we can find deposits of whitish, fibril material in the anterior segment and chamber angle. It can be aggressive. We can usually find pseudoexfoliation material on the surface of lens, but also in the conjunctiva, wall of a short posterior ciliary artery, in eyelid skin,2 as well as in other extraocular structures (extraocular rectus and oblique muscles, vortex veins and optic nerve sheaths).
When treating POAG our primary goal is to normalise intraocular pressure (IOP) and to maintain it this way. It can be achieved by using laser trabeculoplasty that is an effective painless method of lowering IOP. It is known that 56–80 % of patients have 25–30 % lower IOP in period of two years after trabeculopasty in comparison to IOP before treatment.3–5 After 3–5 years a fading effect on IOP is seen in some patients.6–8 When comparing eyes treated with trabeculoplasty and those treated with topical medication, it is seen that eyes treated with trabeculoplasty have better results regarding IOP, visual field and optic disc status.9 Information provided from Advanced glaucoma intervention study (AGIS) publications show that in African Americans when maximum medical therapy have no results the first choice of following procedures is argon laser trabeculoplasty (ALT) and for Caucasians it is trabeculotomy.10 If laser trabeculoplasty is performed in patients with PAOG together with topical medication there is 50 % lower risk of progression.11 Success of laser trabeculoplasty in PAOG is 77 % after two years and 67 % after both five and eight years. In XFG, success after two, five and eight years is 80, 54 and 36 %, respectively.12,13
Laser Trabeculoplasty
Laser trabeculoplasty is used in treatment of POAG, XFG and pigmentary glaucoma. It is not used in treatment of angle-closure glaucoma, secondary glaucoma, juvenile glaucoma and in patients who are under 40 years of age if they do not suffer from pigmentary or XFG. There are several types of laser used for trabeculoplasty: argon laser trabeculoplasty (ALT), diode laser trabeculopasty (DLT), Krypton laser trabeculoplasty and Q-switched Nd:YAG which is also known as selective laser trabeculoplasty (SLT). Regarding ALT we can find three theories explaining the way it works. First of them is Wise and Witter and it is purely mechanical.14 It says that, at the site of laser application, there is shrinkage of the meshwork which causes contraction of collagen in trabecular lamellae. It results in reduction of ring diameter and tightening of trabecular meshwork (TM)which together leads to opening of intratrabecular spaces between laser sites.14–16 According to second theory there is trabecular cell replication and repopulation of the meshwork with fresh trabecular endothelial cells (these cells normally do not have a potential to divide).15 It is presumed that these new cells have more normal physiological function.17 The third theory uses the release of cytokines at the site of laser application in its explanation. This induces matrix metalloprotease enzyme synthesis and chemotactic or vasoactive factors: interleukins 1A and 1B, tumour necrosis factor-alpha. This process attracts polymorphonuclear leucocytes to the affected zone and help in removing the debris from intratrabecular spaces.17,18 Increased turnover of the extracellular matrix is achieved in this way. Argon laser trabeculoplasty as well as SLT causes the recruitment of macrophages and remodelling of extracellular matrix of TM.19 In terms of lowering IOP one year after the treatment, ALT and SLT have equal results.20,21 Diode laser trabeculopasty and ALT are equally effective in lowering IOP over a 5-year period.22 After laser trabeculoplasty membranes are formed in 50–61 % which may be the reason for fading effect on IOP.16 Two studies showed that SLT did not cause thermal damage and membrane formation.18,23 It also minimises trabecular damage. This is because SLT delivers 80–100 times less energy in pulse mode and that is under the thermal relaxation time of trabecular tissue. It targets pigmented TM cells, but it does not cause structural damage of TM.18 Regarding side effects of laser usage we can say that they are not frequent and they usually appear in the form of transient IOP increase, intraocular inflammation, iritis, haemorrhage, thermal burns of corneal epithelium, formation of anterior synechia and visual field defects.18 The purpose of this study was to evaluate DLT efficacy in lowering IOP in patients with POAG and XFG. The aim of the study was to find the minimum time after DLT that showed a decrease of IOP and to establish the maximum IOP decrease after which no further changes were expected.
Table 1: Intraocular Pressure Decrease Compared with Baseline Values and Between POAG and XFG
Material and Methods
A one-year, open-labelled, controlled, prospective study was conducted between November 2007 and November 2009. Efficacy of DLT in lowering of IOP was compared in patient with POAG and XFG. Twenty patients with XFG (33 eyes) and 20 patients with POAG (36 eyes) were enrolled in this study. All patients provided informed consent. The study was approved by Ethical Committee, Medical Faculty of Novi Sad, Serbia, 2007. Inclusion criteria were male and female aged 30 years or more with previously diagnosed XFG and/or POAG. They had to be using not less than one and no more than three topical anti-glaucoma drugs (prostaglandin analogues, β-blockers, α-agonists or carboanhidrase inhibitors). They had to have average IOP value of 19–30 mmHg in at least two consecutive IOP measurements at 8 AM in previous two months. Eligible patients were enrolled in the study in a consecutive manner. Medication was not changed in follow-up period. None of the patients enrolled in the study had previous laser trabeculoplasty.
Exclusion criteria were the following: no visual acuity (no light perception), angle grade measured by gonioscopy less than two (Shaffer classification), cup/disc ratio greater than 0.9, a history of chronic and recurrent inflammatory eye disease, severe retinal disease,or any abnormality of the cornea which prevented reliable applanation tonometry; and/or decrease of transparency and ocular trauma as well as previous filtering or cataract surgery. Patients with IOP greater than 21 mmHg in period of 30 days after DLT were also excluded because of potential safety risks. The additional exclusion criteria were pregnancy; unstable or uncontrolled cardiovascular, hepatic and renal diseases; history of hypersensitivity to α-agonists. The best corrected visual acuity (logMAR scale), biomicroscopy, gonioscopy, detailed fundus examinations, c/d ratio and bilateral IOP measurements at 8 AM using Goldmann applanation tonometry, all were conducted. As a topical premedication, α-agonist brimonidine 0.1 % (Alphagan(R)) has been applied 40 minutes before the intervention. DLT was performed with the Zeiss Visulas 532 s diode pumped solid state laser system, 532 nm, 100 μ laser spot, 0.1 second single emission of 600–1,200 mW. Using 12 x biomicroscopy magnifications we applied, through gonioscopy lens, the laser beam on the upper third of TM. On the inferior 180 degrees of TM DLT was performed. There were always 40 to 50 burns and the space between two of them was 100 μ. Dexamethasone 1 % (Maxidex(R)) q.i.d., was applied to prevent a potential inflammatory reaction seven days after DLT in all patients. Safety and efficacy evaluations were performed on day seven then on one, three and six months, one year after diode laser trabeculopasty. IOP was measured at 8 AM.
Observers were masked when measuring IOP. All ocular side effects were documented (blurred vision, ciliary hyperaemia, iritis, elevated IOP). For statistical analysis we used Microsoft Excel software with standard statistical parameters and methods – numerical data were presented using MIN, MAX and average values; standard deviation (SD); and a 95 % confidence interval (CI). Student t-test was used to make comparison between POAG and XFG groups and to compare IOP values inside the groups.
Results
The results of this study were the following: two of 40 patients were excluded because they did not show up on scheduled control. Other 38 patients were aged 70.1 Å} 9.1 in POAG group and 67.9 Å} 11.4 in XFG group (X ± 2SD). There were no significant differences in age and other demographic characteristics between these two groups (p=0.19), as well as in gender (p=0.24) and best corrected visual acuity (p=0.51). The horizontal and vertical c/d ratio did not show any statistically significant differences (p=0.52 and p=0.41, respectively). Regarding baseline IOP (see Figure 1) it was 22.8 ± 2.1 mmHg for POAG group and 23.7 ± 2.6 mmHg for XFG (p=0.49 – no statistically significant difference). Measurements of IOP in POAG showed the following results: on day seven it was 17.9 ± 1.9 mmHg which is 21.2 % decrease from the baseline (see Table 1), on day 30 it was 16.1 ± 2.4 mmHg which is 29.4 % decrease from the baseline, after 3 months 16.0 ± 2.5 mmHg that is 29.8 % decrease from the baseline, after six months 15.5 ± 2.7 mmHg or 31.9 % decrease from the baseline and after one year 16.3 ± 2.9 mmHg that makes 27.9 % decrease from the baseline. The results in XFG group were: mean IOP on day seven was 16.8 ± 2.1 mmHg or 26.9 % decrease from the baseline, on day 30 it was 14.3 ± 2.2 mmHg which is 38.3 % decrease from the baseline, after 3 months 13.9 ± 2.4 mmHg (39.0 % decrease from the baseline), after six months 13.8 ± 2.7 mmHg or 39.9 % decrease from the baseline and after one year 15.1 ± 3.1 mmHg that makes 36.3 % decrease from the baseline. During one year of follow-up period IOP was significantly lower compared to baseline IOP levels (p≤0.01). On day seven, month one, month three, month six and one year, statistically significant differences were found between the two groups (p=0.02), (p=0.058), (p=0.02), (p=0.002), (p=0.05) respectively. In both groups, at each visit in period from one month after DLT to one year after DLT , IOP was significantly lower (p≤0.01) compared to baseline IOP levels. There were no related adverse effects throughout the follow-up period in this study.
Conclusions
The efficacy and safety of DLT was evaluated in patients with POAG and XFG in the prospective study. No IOP decrease after DLT until three months after procedure was seen in only three out of 69 eyes. By the end of follow-up period, the IOP-lowering effect of DLT was significant in both groups compared with baseline values. In POAG group it was 27.9 % (p<0.01) and in XFG group it was 36.3% (p<0.01). After 3 months the success of DLT was 9.2 % greater in XFG group than in POAG group (p=0.002) which is in accordance with other studies.24,25 The predictive final decreased value of IOP might be evident on day 30, which is a longer period than stated by other authors who showed the predictive IOP values on that day.26–28 regarding both groups as open-angle glaucoma, it is shown that a mean IOP decrease is 34.4 % after three months. In the Early Manifest Glaucoma Trial (EMGT) it is reported that there was a 25 % of IOP decrease from the baseline at three months. The difference is because our study had higher percentage of patients with XFG than EMGT. The results of this study are in accordance with previous findings which state that lower baseline IOP predicts lower post-treatment IOP especially in patients with XFG. There is no age or sex dependence on DLT efficacy. This study confirmed that diode laser trabeculoplasty is an effective and safe method of treatment for patients with open-angle glaucoma. Its outcome could be predicted as early as day seven of the follow-up period. It is more successful in pseudoexfoliative glaucoma than in other open-angle glaucomas.