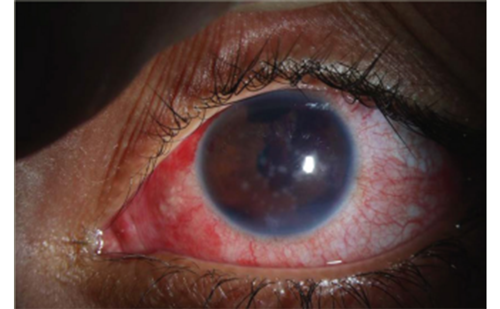
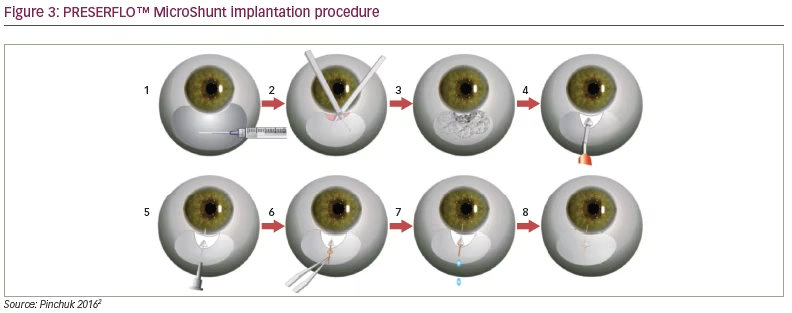
Although for open-angle glaucoma the level of intraocular pressure (IOP) is no longer recognized as a defining criterion, it is a major risk factor for the development and progression of the disease.1–6 Medical, laser, and surgical therapies therefore reduce IOP to attempt to modify disease progression.7,8 Trabeculectomy is the current gold standard of filtration surgery in the management of primary open-angle glaucoma following the failure of IOP-lowering medications or non-invasive surgery such as laser trabeculoplasty.9–11 Trabeculectomy can effectively control IOP,12–15 even in the long term,16–20 but published success rates can vary, in part due to the lack of standard definitions of success.21 Moreover, trabeculectomy is associated with significant complications including early post-operative hypotony, bleb leak, blebitis and bleb failure, choroidal effusions, endophthalmitis, hyphema, shallowing of the anterior chamber, and accelerated cataract progression.9 Patients who fail to respond to trabeculectomy may require additional surgery, in some instances a second trabeculectomy, or implantation of a drainage device.22 As a result, some studies have suggested that the risks of trabeculectomy outweigh the benefits.18,23
Incremental improvements in trabeculectomy have proved valuable in refining the technique and include the use of a traction suture to control the position of the eye, appropriate and optimal wound healing techniques to prevent fibrosis and scarring, use of a fornix-based conjunctival flap, creation of a large scleral flap to maximize posterior aqueous flow and enable the development of a diffuse bleb, adjustable sutures to control aqueous flow, and a standardized trabeculectomy aperture.24,25 Such refinements can improve patient outcomes.26,27
To view the full article in PDF or eBook formats, please click on the icons above.