With increasing patient expectations and cataract surgery being regarded as a refractive procedure, multifocal intraocular lenses (IOLs) are one of the most effective ways of achieving a good visual acuity at distance, intermediate and near. However, precise biometry and astigmatism correction must be considered in order to achieve spectacle independence.
It is well documented that the presence of astigmatism in eyes with a multifocal IOL compromises visual acuity.1,2 Corneal astigmatism over 1.25 dioptres (D) is present in up to 29% of patients subjected to cataract surgery.3,4 For astigmatic correction during cataract surgery, toric IOLs are more effective and predictable than other techniques, namely corneal incisional techniques, especially for higher degrees of astigmatism.5,6
Several multifocal toric IOL designs are available today, including bifocal, trifocal and enhanced depth-of-focus (EDOF) lenses.
In a recent study,7 we investigated the visual performance and patient satisfaction with the Tecnis multifocal toric IOL (Tecnis ZMT, Abbott Medical Optics, CA, US), a diffractive toric IOL which provides a +4.0 D near addition and a 50/50 light distribution to the distance and near foci. In this prospective case series of 60 eyes with a 6-month follow-up, the Tecnis multifocal toric IOL offered good visual outcomes, with an excellent visual acuity for far and near and functional visual acuity for the intermediate distance. The mean uncorrected distance visual acuity was 0.07±0.1 LogMAR, the mean uncorrected intermediate visual acuity was 0.18±0.09 LogMAR and the mean uncorrected near visual acuity was 0.03±0.09 LogMAR. The refractive predictability was very good, with the spherical equivalent refraction within ±0.50 D of the attempted correction in 93% of the eyes. Refractive cylinder was within ±0.50 D in 77% of the eyes. The IOL position was stable postoperatively (mean toric IOL axis rotation 3.18±3.28 degrees at 6 months).
Unwanted photic phenomena (halos, glare, starbursts, ghost images and diplopia) are intrinsic to the design of diffractive multifocal IOLs due to the edges of the steps of different ring zones producing the phenomena.8 In our study, we asked patients to rate these phenomena in a 0–5 Likert scale. The most frequent visual disturbance score was 1/5 (minimal trouble). No patient reported a score of 4 (overwhelming trouble). Although in our series all patients were spectacle independent, the results may have been limited by the sample size.
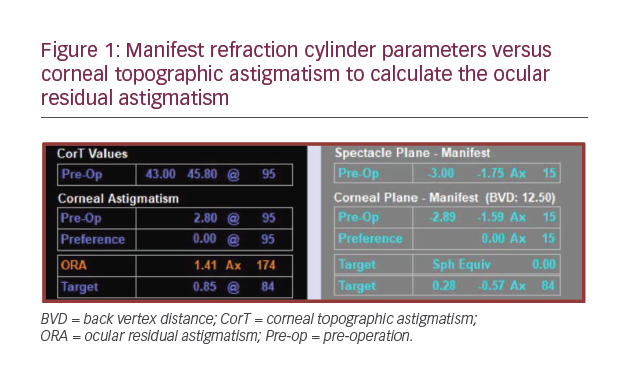
Since our Tecnis ZMT study, with the recognition of the importance of including the posterior corneal astigmatism in toric IOL calculation in order to achieve precise results, several new toric calculators have been developed. The AMO toric calculator has been updated to include the option of considering the posterior corneal surface in the calculation. As we have shown recently, this may allow for even better outcomes with toric IOLs, with minimal residual astigmatism.9
A precise calculation must be combined with a precise surgery, with a well-centred capsulorhexis with complete overlap of IOL optic, and a digital marking technique or intraoperative aberrometry for precise IOL alignment.
Trifocal IOLs, with the addition of an intermediate focus, may have better visual results for the intermediate distance and EDOF IOLs allow a good intermediate vision and some degree of near vision with the advantage of having a better tolerance to residual refractive error and a lower incidence of photic phenomena.10–12
With the recent developments, multifocal toric IOLs are an essential piece of the armamentarium of a refractive cataract surgeon. As with any multifocal IOL, managing of patient expectations, precise data gathering, meticulous ophthalmologic examination and surgical skills are the keys to good results and patient satisfaction.