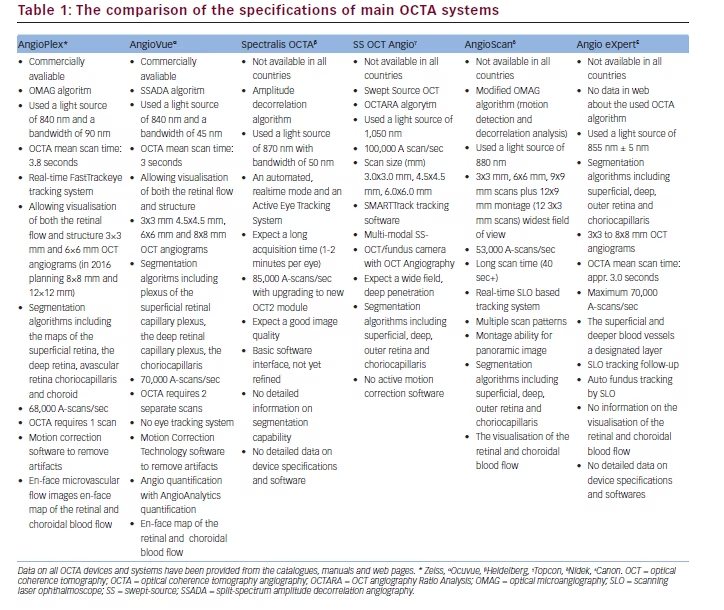
Glaucoma is a chronic progressive optic neuropathy, which can lead to irreversible blindness.1 It is characterized by loss of retinal nerve tissue that results in visual function deterioration. Structural changes, such as accelerated loss of retinal ganglion cells (RGCs) and their axons, and a specific pattern of damage in the optic nerve head (ONH) associated with visual field (VF) loss, are considered hallmarks of glaucoma.2
The efficacy of glaucoma management depends mostly on the ability to reliably detect disease progression as early as possible. Detection of progression allows the clinician to initiate or modify treatment, which can slow glaucoma progression and potentially preserve vision.
Even though optic disc stereophotographs are considered the gold standard for the evaluation of glaucomatous structural damage, the estimation of structural progression in glaucoma using this tool is challenging due to its subjective nature.3 The recent evolution of imaging tools noticeably improved the objective and quantitative determination of structural changes and the assessment of progression caused by glaucoma.4–6 However, the assessment of structural progression in glaucoma still comprises several dilemmas due to difficulties in differentiating between true glaucomatous change and natural agerelated loss of retinal nerve tissue, measurement variability, and a lack of widely accepted and efficient gold standard criteria for establishing glaucoma progression. In this review we will summarize the imaging tools that are currently available, namely scanning laser polarimetry (SLP), confocal scanning laser ophthalmoscopy (CSLO), and spectral domain optical coherence tomography (SD-OCT). We will focus particularly on their ability to detect glaucoma progression, as well as the strengths and limitations of each imaging technology.
Detection of Glaucoma Progression
Progression of glaucoma can be estimated by subjective assessment based on clinical experience and judgment, or by statistical analysis of quantitative measurements. The statistical methods used to detect glaucoma progression can be classified as event- or trend-based analysis.
In event-based analysis a series of follow-up measurements are compared with baseline measurements, and progression is defined when measurements exceed a predetermined threshold for change from baseline. This method is highly sensitive to the threshold level, with a higher threshold resulting in fewer cases identified as progressing with only a small number of false positive classifications and vice versa when choosing a lower threshold. The threshold is often selected based on the physical properties of the imaging device (e.g., measurement reproducibility), or by population-based data. The main disadvantage of this method is the effect of erroneous deviating measurements that might be labeled as progression. A confirmatory second test can resolve most of the false progression classifications in this method.
Trend-based analysis uses regression analysis or mixed effect regression analysis to estimate the rate of change in the examined parameters. Progression is defined either when the rate of change is significantly different than a no change slope (zero slope), or when the rate is different than population or individually derived slope. This method is less affected by measurement errors at a given time point than the event-based method, but it requires a large number of tests in order to be considered reliable. As this method provides a slope, this can be extrapolated to predict future progression and risk for the development of functionally significant visual deficits, thus impacting glaucoma management. The main disadvantages of trend-based analysis are the requirement for a large number of visits and the risk for ignoring true progression events when changes initially occur. The last disadvantage is due to the neutralization of sudden progression events by the overall rate of change. This can lead to a delay in identifying progression that would lead to the inappropriate management of glaucoma. Moreover, the basic assumption for trend-based analysis is that progression is a linear process, which might not be true for all eyes.
Another approach for the detection of progression is using permutation analysis while assessing the parameters of interest.7 In this method, the chronologic order of the measurements are randomly shuffled and compared with the actual rate of change over time. The advantage of this method is that it uses individual subject measurements in order to define the measurement variability rather than relying on population-based information, which might best reflect the actual disease behavior for given patient. However, this method also requires a large number of tests in order to provide reliable limits.
Confocal Scanning Laser Ophthalmoscopy
CSLO is a noninvasive imaging technology that uses a 670 nm wavelength diode laser and confocal optics to obtain high-resolution threedimensional (3D) images of the ONH region. The built-in software merges the stacks of acquired parallel scans into a 3D image, and determines the height of the surface along the optic disc and peripapillary retina. After the operator marks the ONH margin, the device can compute a variety of stereometric parameters, including disc area, rim area and volume, cup-to-disc ratio, etc. The device can also generate fully automated structural measurements by fitting the pre-defined configuration of the ONH region to the scan.
The most recent commercially available CSLO device is the Heidelberg Retina Tomograph III (HRT III; Heidelberg Engineering, Heidelberg, Germany). Previous studies have shown rim area to be the most repeatable parameter, both with between-visit and between-operator variability, and it has demonstrated good longitudinal reproducibility.8–10 Therefore, this parameter is often considered to be the best candidate among the stereometric parameters provided by the device to identify and track glaucomatous changes.
The topographic change analysis (TCA) is currently the primary algorithm for assessing glaucomatous progression available in the HRT III. It is an event-based analysis that identifies topographic surface height change exceeding a predefined threshold level across the entire scanned area of the ONH and peripapillary region. TCA estimates significant and repeatable changes at the superpixel (4 × 4 pixels) level using the analysis of variance technique, and displays results in a color-coded map, with red indicating depression and green indicating elevation compared with baseline (see Figure 1). The location of the labeled clusters should be considered when evaluating the TCA report. Clusters within the boundaries of the ONH should be considered primarily, while clusters along blood vessels should be ignored as they are mostly induced by vascular pulsation.11
The concordance between the TCA analysis and optic disc stereophotography in the detection of glaucoma progression varies from 65 % to 82.3 % as reported in different studies.12–14 Some studies reported that TCA analysis detects glaucoma progression earlier than VF11 and SD-OCT retinal nerve fiber layer (RNFL) thickness examination,15 although more than 70 % of TCA progressors did not progress by VF during a 6-year-long follow-up period16 while nearly 40 % of TCA stable eyes showed optic disc stereophotographic or VF progression.17
For a median follow-up period of 4.0 years, sixty-one stable glaucomatous eyes were prospectively followed. During this period the participants had periodical HRT imaging and VF and optic disc photography.17 During the follow-up period, 38.4 % of the eyes that were defined as TCA-stable showed VF and/or photographic progression while only in 22.9 % of eyes that were labeled as TCA-progression there was evidence of VF or photographic progression. This discrepancy might indicate a limited performance of this method or the often observed discordance between progression detected among different analysis methods.
Spectral Domain Optical Coherence Tomography
SD-OCT obtains real-time, high-resolution, cross-sectional tissue scans at the micrometer scale. This iteration of the technology is based on analyzing the frequency information of back reflected light from the eye generated by a near-infrared broad-bandwidth light source that is detected by a charge-coupled device (CCD) camera and a spectrometer.18 The frequency information is converted into intensity profiles using Fourier-transformation, allowing the acquisition of cross-sectional scans of tissue with rapid scanning speed. Fast scanning rate (currently, up to 75,000 axial scans/sec) allows swiping through the area of interest to acquire 3D data. The glaucoma module obtains RNFL thickness data from a 3.46 mm diameter peripapillary circle centered on the optic disc, peripapillary RNFL thickness map, and ONH measurements.
There are several commercially available SD-OCT devices, and at the time of writing only some of them offer built-in progression analysis software: the Cirrus HD-OCT (Carl Zeiss Meditec, Dublin, CA), Spectralis OCT (Heidelberg Engineering, Heidelberg, Germany), RTVue Premier (Optovue, Fremont, CA), and Topcon 3D OCT-2000 (Topcon, Tokyo, Japan). All these devices perform trend-based progression analysis, using linear regression, to compute the rate of change of RNFL thickness (global or regional) over time. This rate of change can also be used to predict future progression beyond the most recent visit, and allows the clinician to set goals for treatments.
Currently, only Cirrus HD-OCT and Spectralis OCT provide event-based analysis (the principles of this method were explained above) in addition to the regression analysis. The guided progression analysis (GPA) of Cirrus HD-OCT estimates disease progression by both event- and trendbased analysis. Event analysis is performed on RNFL thickness and change maps (see Figure 2a) and the circumpapillary RNFL thickness profiles (see Figure 2c). Locations where RNFL thickness was thinner than baseline beyond the level of the population-derived reproducibility error are highlighted. In the uppermost panel (see Figure 2a) two baseline (left) and two final exams (right) are presented. The full sequence of scans acquired over the period of follow-up is presented in the bottom panel (see Figure 2e). Color-coded results on the RNFL thickness change map and the RNFL thickness profiles mark the first occurrence of statistically significant change in yellow, while consecutive RNFL thinning in the same location is shown in red. It should be noted that in the case presented in Figure 2, a significant change was initially detected in visit #3, and therefore the area marked in the inferior region (see Figure 2a) is labeled in red in both of the last visits (right). The trend analysis for RNFL thickness change (overall and in hemifields) and the ONH’s cup-to-disc ratio over the course of the follow-up period are reported in Figure 2b.
The RNFL Change Report of the Spectralis OCT provides event-based analysis of circumpapillary RNFL thickness profiles and trend-based analysis of average and sectoral circumpapillary RNFL thickness. The analysis uses the same color code (yellow for the first event and red for the next consecutive event in the same location) to show significant progression from baseline.
SD-OCT has been shown to be more repeatable and reproducible than the earlier generations of the technology, time-domain OCT (TD-OCT),19–23 and optic disc stereophotography.24 This enables the identification of smaller structural changes with higher confidence and improves the ability to detect changes.25
A longitudinal study of 186 glaucomatous eyes reported that the most common pattern of RNFL progression was the widening of RNFL defects, followed by the development of a new RNFL defect, and then a deepening of preexisting defects.26 Therefore, the ability of SD-OCT to provide information from the entire peripapillary region further improves the chances of detecting progression. The same study revealed that RNFL progression most commonly occurs in inferotemporal meridians at 2 mm from the optic disc center, which supports the observation that the superonasal VF frequently deteriorates faster as glaucoma progresses.27
SD-OCT technology showed poor agreement with optic disc stereophotography and VF testing in the detection of glaucoma progression,25,28,29 similar to TD-OCT,30–32 which might be due to spatial A retrospective study of 272 glaucomatous eyes evaluated the performance of Cirrus HD-OCT GPA for detection of glaucoma progression.33 Expert assessment of optic disc photographs, VF GPA, or VF index linear regression analysis were used as reference standards of progression. The authors reported a sensitivity of 25 % and specificity of 88.61 % for the GPA. At the time of this writing there are no published studies on the performance of the automated progression algorithms of other commercially available SD-OCT devices.
Scanning Laser Polarimetry
SLP measures RNFL thickness by scanning the retina with a polarized laser beam, which splits into two components while passing through highly organized and parallel structures, such as the RNFL.34 These components travel at different velocities, which creates a relative phase shift (retardation). The amount of retardation is proportional to the thickness of the birefringent tissue, thus allowing the instrument to measure the RNFL thickness.
The most recent commercially available SLP instrument, GDx PRO (Carl Zeiss Meditec, Dublin, CA), uses GPA software for the detection of glaucoma progression, similar to the one described above for Cirrus SD-OCT (see Figure 3). The GPA provides both event- and trend-based analyses of RNFL thickness change over a follow-up period. The software can provide two types of analysis, depending on whether one or three scans are obtained at each visit. The “fast mode” compares the two most recent images with the two baselines: change is identified as significant if it exceeds the predetermined measurement variability based on population-derived data. By contrast, the “extended mode” uses a mean of three images at each visit, and identifies significant change based on the measurement variability computed with the permutation analysis described above.
GDx’s GPA Image Progression Map and the Temporal – Superior – Nasal – Inferior –Temporal (TSNIT) Progression Graph (see Figure 3a) represent an RNFL thickness event-based progression analysis using the same color-codes as in Cirrus HD-OCT. In the bottom part of the printout all the exams from the follow-up period are presented (see Figure 3c). Linear regression analysis of mean and hemifield RNFL thickness are presented in Summary Parameters Charts (see Figure 3b).
At the time of writing, there are no published data on the agreement of current generation GDx GPA software with ONH stereophotography or VF examination in detection of glaucoma progression. An observational cohort study of 453 glaucoma, glaucoma suspect, and healthy eyes with mean follow-up of 46 months examined the performance of GDx GPA for detecting glaucoma progression.5 Progression was defined by VF GPA and expert evaluation of optic disc stereophotographs. Out of 34 eyes that showed progression by VF and/or optic disc stereophotographs the GDx GPA detected 17 eyes (50 % sensitivity). Fourteen eyes showed progression by GDx GPA for a specificity of 96 %.
Conclusion
Although the imaging tools currently available have shown the capacity to detect and quantify glaucomatous progression, the estimation of glaucoma progression remains clinically challenging. This is due to the variable course of the disease and its slow progression, the lack of a commonly accepted gold standard that can be used to accurately indicate glaucomatous progression, and the device measurement variability when used in serial assessments. Additionally, age-related reduction of peripapillar and macular RNFL thickness30,35,36 should be considered while assessing glaucoma progression. As the ability to detect disease progression and the full spectrum of disease severity varies between structural and functional methods, it is recommended to clinically assess progression with both methods.30,37