Presbyopia-correcting intraocular lenses (Pr-C IOLs) can provide a full range of visual corrections for far, intermediate and near vision. It is important to evaluate the outcomes from Pr-C IOLs in order to improve our results. Experience has taught us to test for certain parameters that best correlate with the patient’s real-life visual performance and satisfaction. We have developed a system to collect important pre- and post-operative data to accurately access Pr-C IOLs’ effectiveness. The first parameter is the patient’s visual acuity. The minimum size letter that a person can resolve at near distance is an important measure of their near vision. It is important to standardise the measurement, which has been performed well for distance acuity, but not for near acuity. The latter is regularly reported in Snellen or Jaeger number formats in the US, N numbers in the UK and Parinaud numbers in France. Due to these differing systems, no comparisons can be drawn among different studies. Our experience has also shown that patients often require a print size two or three times larger than their peak near acuity limits before they can achieve their maximum reading speed. It would be useful to have a standardised method of measuring near vision that was more easily translatable into other formats.
The second parameter to consider is reading speed. In our experience, it is common for a patient not to be able to comfortably read a print of the same size as to what vision tests show their minimum resolvable print size to be. Patients usually ask for a print size that is significantly larger than their minimum resolvable letter size. Reading speed is an objective measure of reading performance. Questions regarding how patients perform in different everyday life activities are too subjective for comparisons (i.e. “How is your vision while shopping?”). This is simply a too general question, which does not allow for useful comparisons among different patients, or among the same patient’s sequential exams. The third parameter is depth of focus. Different IOLs can be expected to perform differently at different distances when reading. The defocus curve is a very useful piece of data for us to better understand the visual performance of a specific IOL: if a Pr-C IOL is found to have a predictable defocus curve, this information can be valuable for the patient’s selection and counselling. The fourth parameter to evaluate is the patient’s spectacle dependency after surgery. This is a rather objective criterion – if someone does not ever use glasses, this is a very definite end-point. Likewise, the presence or absence of photic phenomena is important. Although, rather than having the patient respond either yes or no, it is much more indicative to quantify the amount and severity of these events.
Overall, we have attempted to estimate patient’s satisfaction with various IOLs through questionnaires that present simple questions in terms of quality of life and vision. Unfortunately, these questionnaires are quite boring for our patients, and they do not give us clear feedback on real visual performance in their day-to-day life.
Introducing the Eyevispod™
We have attempted to solve these problems with a new system to measure, collect, record and analyse near vision data. Early on, we understood the need for an objective measurement system that could record data as it was collected. We therefore have developed a diagnostic machine – the Eyevispod™ – which can study all of these parameters. In our experience it has proved to be useful to us and our patients.
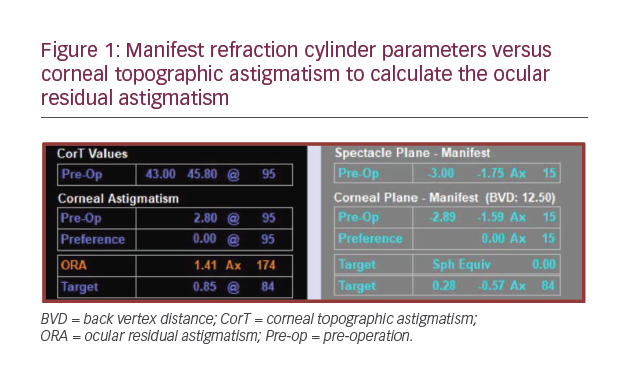
The Eyevispod is a computerised system that allows the convenient measurement, collection and recording of a detailed assessment of near and intermediate visual performance in patients with or without Pr-C IOLs. It overcomes the limitations of traditional visual acuity charts, by presenting the patient with a standardised image and recording the results as soon as they are measured (see Figure 1).
The traditional system of measuring peak near acuity does not correlate well with real-life reading vision. It cannot take into account the variety of day-to-day situations, such as shopping, going to restaurants or driving. Furthermore, traditionally, we have had no way of objectively measuring and documenting common symptoms, such as glare and halos, during our routine examinations.
The Eyevispod system performs a comprehensive assessment of near and intermediate visual function and gives a score (as a per cent of normal) of the patient’s visual performance. By simulating the most common daily visual tasks and problems on a tablet PC and by processing the data from a series of subsequent tests, the Eyevispod (previously called SlowFast) creates a functional score of the pre- and post-operative near vision. This score is useful for practical and medico-legal purposes. It can also be used to compare the outcomes of various surgeries for presbyopia (multifocal IOLs, accommodative IOLs, conductive keratoplasty, scleral bands or laser keratorefractive surgery).
The system is easy to use, relatively time-efficient (a five-minute time test) and the results are easily understandable. Patients hold the tablet PC in their hands and select the answers with the tip of a pointer on the touchscreen.
Tests that are featured in the device are EyeVisPod tests, near visual acuity measurement, reading speed and comprehensive test, social reading quality, photic phenomena calculator and automatic defocus curve. The tests are usually administered sequentially.
First, near visual acuity is measured with the patient positioned 40cm away from the screen. A series of progressively smaller letters are shown and the patient stops when no longer able to read them (see Figure 2). The size of the letters is presented in multiple systems simultaneously. They are shown inside the red ellipse. This value is recorded by the Eyevispod.
The next test is reading speed. The program comes in seven languages and reading passages are rated as low, medium and high difficulty. Once the patient begins reading the passage, a stopwatch on the Eyevispod is started and then stopped at the end of the passage. The reading speed is then automatically calculated and recorded. Afterwards, the patient is asked a series of questions to estimate their comprehension of the passage. We believe that measuring reading speed in such way is the best measure for near vision performance (see Figure 3).
Measuring reading speed without testing reading comprehension can be misleading; transmitting information to the brain is an essential task of visual function. If we do not test comprehension, we would not know whether the patient was rushing his or herself for the test, without actually allowing enough time to comprehend what they were reading as they would in a real-life situation. What we really want to assess is the functional everyday reading speed, which is that speed at which the patient is able to still concentrate enough to understand the text.
The next test is a series of everyday visual tasks that are often problematic for presbyopic patients. Standardised images are presented on the tablet PC, both pre- and post-operatively. Several examples of these commonly problematic objects are reproduced on the screen and divided into three categories: near vision (reading newspapers), intermediate vision and photopic phenomena.
In the near vision category, there is an entire set of near images devoted to newspapers. It includes titles, subtitles, body text, different paper colours and the ‘financial section’, in which numbers and tables are usually printed in the smallest fonts. The intermediate vision category contains examples of images from intermediate distance daily tasks. These include a full-size car dashboard, door plates, price tags, nutrition information labels, road maps and a music score (see Figure 4). All are actual size images, which allow us to directly test the patient’s everyday social visual performance at both near and intermediate distances. In the last category, diffractive images and aberrations are simulated with various degrees of severity. Patients select the images that most closely replicate their own night vision (see Figure 5). A contrast sensitivity test can also be performed with Eyevispod system (see Figure 7). A final layout of all the tests performed with a functional global score can be obtained and printed, as well as for each single test (see Figure 8). As these tests are completed, the data is recorded and eventually reported on a numeric scale out of 100.
The final section of the test allows for the creation of a monocular or binocular defocus curve. These curves can be compared with those obtained from other patients using the same standardised testing methodology. Capturing and comparing data in such a way allows us to really compare the functional quality of vision after an IOL is implanted (see Figure 6).
Towards Standardised Evaluation of Intraocular Performance
In conclusion, the Eyevispod provides us with a complete profile of both the visual acuity and quality (including near vision) of the patient and an assessment of unwanted visual images. With just one single testing system, we can measure the patient’s overall real-life visual performance. Results are then automatically archived in the digital database included in the programme. This cumulative database can then automatically characterise a range of typical outcomes for any given IOL.
Finally, by testing patients both pre- and post-operatively, we can obtain a true objective measure of how much their visual performance has improved, or how many other visual symptoms have worsened after IOL implantation.
Although it has been advocated for many years, standardised outcome testing has become increasingly critical, as we continue to have many new and different IOLs and procedures to scientifically compare. We are confident that this improved and high-tech way of testing patients’ visual outcomes will lead to a greater standardisation of clinical methods traditionally used to measure near acuity. ■