Branch retinal vein occlusion (BRVO) represents a common retinal vascular disease, with a cumulative 15-year incidence of 1.8% in the overall population.1 With regard to its association with cardiovascular diseases (particularly arterial hypertension and ischaemic heart disease),2 the diagnosis is of major relevance. As a quick and noninvasive method, optical coherence tomography angiography (OCT-A) nowadays facilitates diagnosis and follow-up of affected patients.3 Optimal control of the cardiovascular profile is of utmost importance,4 yet no beneficial effect of anti-aggregating platelet therapy or systemic anticoagulation on the visual outcome in patients with BRVO has been shown.5 BRVO is often accompanied by macular oedema (ME) and may lead to secondary neovascular complications (in up to 28.6%).6 Thus, BRVO represents a serious, vision-threatening entity. However, according to Gutman et al., 25% of patients present with transient ME followed by spontaneous resolution.7 ME occurs due to endothelial damage and hypoxia, which results in an inflammatory response, with subsequent up-regulation of inflammatory mediators such as tumour necrosis factor-alpha, prostaglandins, leukotriens, integrins and vascular endothelial growth factor (VEGF).8,9 Particularly, the marked rise of VEGF levels in BRVO patients has been studied intensively.10,11
Historically, observation, lasercoagulation or surgical treatments (radial optic neurotomy, retinochoroidal anastomosis, arteriovenous (AV) sheatotomy) represented the only available therapeutic options.
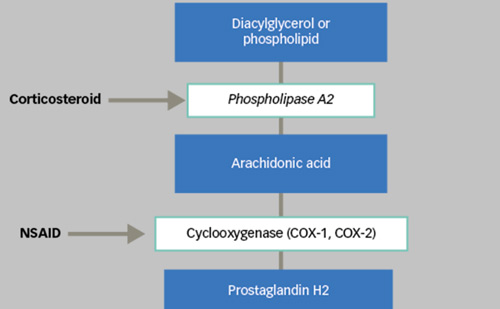
The advent of anti-VEGF agents in recent years has revolutionised the treatment options for BRVO. Three different anti-VEGF agents are available for intravitreal administration: bevacizumab (off-label), ranibizumab and aflibercept. Given the impressive results of major clinical trials,12,13 anti-VEGF drugs rapidly became the gold-standard therapy for BRVO associated ME. Further pharmacotherapeutic options include intravitreal corticosteroids (triamcinolone/off-label; dexamethasone). The effectiveness of a dexamethasone implant has been evaluated in the SCORE and GENEVA trials.14,15 The rationale for intravitreal steroids for the treatment of RVO-associated ME is related to the inflammatory reaction involved in the pathogenesis of ME. Besides VEGF, a significant rise of diverse cytokines and chemokines in ocular fluids of BRVO patients has been demonstrated.16 In contrast to specific anti-VEGF compounds, corticosteroids inhibit a whole panoply of growth factors, chemokines and cytokines associated with ME. Nevertheless, the wellknown adverse effects on intraocular pressure and cataract formation should be considered.17
Despite the variety of treatment options, we are confronted with several questions:
• Which drug should we use? Is any anti-VEGF agent superior?
• Does long-term treatment with anti-VEGF agents affect the retinal circulation?
• Is switching or combining different treatment options beneficial?
• What is the recommended treatment regimen? When should we start, and for how long should we treat?
• Should we add retinal laser to intravitreal pharmacotherapy?
With regard to the comparative effect of different anti-VEGF agents, at this time, no head-to-head studies exist. Although tempting, the comparison of BRAVO (Ranibizumab for the Treatment of Macular Edema following Branch Retinal Vein Occlusion) and VIBRANT (ranibizumab versus aflibercept) trials does not allow conclusions concerning this matter, owing to the deviating study endpoints. A retrospective trial comparing the effect of bevacizumab versus aflibercept in treatment-naïve BRVO eyes did reveal similar efficacy and duration.18
Relating to long-term effects of anti-VEGF agents on the retinal circulation, Mir et al. recently reported a promoting effect on the improvement of retinal nonperfusion in RVO patients following monthly ranibizumab injections.19 This is an interesting aspect, but up to now, no data on longterm (>36 months) observation exist.
As a rationale for combining or switching drugs or therapeutic methods one could mention the risk of cumulative toxicity and tachyphylaxis following repeated monotherapy. Unfortunately, limited evidence for combination therapy exists. Unpublished data (Wirth et al., Aflibercept in Branch Retinal Vein Occlusion – clinical outcome 12 months after changing treatment from bevacizumab/ranibizumab) did show a prolongation of retreatment intervals, as well as beneficial functional and anatomic changes after switching from bevacizumab and/or ranibizumab to aflibercept.
Combination of steroids and anti-VEGF agents may be of significance in recalcitrant ME, but its superiority (over anti-VEGF alone) remains to be elucidated. Likewise, up to now, no studies have evaluated the outcome of anti-VEGF injections alone versus anti-VEGF plus laser photocoagulation. Apart from that, panretinal laser photocoagulation was not found to reduce the total VEGF load in BRVO eyes.20 However, a recent study indicated that the addition of scatter photocoagulation to ranibizumab may reduce progression of retinal nonperfusion in patients with BRVO.19
To summarise, the achievement of a potential synergistic effect by combination of different interventions requires further study.
According to the SHORE and HORIZON studies, there is no superiority in pro re nata (PRN) versus monthly treatment.21,22 The treat and extend regimen represents a popular option in clinical practice and has been shown to reduce treatment burden and associated costs.23 Initiating treatment immediately after diagnosis may provide the highest vision gains.24 Long-term follow-up data from the RETAIN study demonstrated that 50% of eyes still required anti-VEGF injections in regular intervals.25 To date, we have no final answer on the required duration of treatment.
In conclusion, we are fortunate in having a battery of therapeutic methods available. However, for evidence-based management of BRVO, larger comparative studies are needed to conclusively evaluate different therapeutic options as well as their combinations