It has been over five years since riboflavin–ultraviolet A (UVA) corneal collagen cross-linking treatment was introduced.1 Longterm stability of up to six years has been reported for this treatment in stopping the progression of keratoconus (KC).1,2 It is estimated that >1,000 corneal cross-linking (CXL) procedures are performed monthly worldwide.3 Other available treatment modalities for KC include glasses, contact lenses, intracorneal rings, epikeratoplasty and thermal keratoplasty. However, the effect of these treatments is only temporary as they do not stop the progression of KC, and the final choice left is penetrating keratoplasty with many potential intra- and post-operative complications.2
Post-laser-assisted in situ keratomileusis (LASIK) ectasia, reported since 19984 and characterised by progressive corneal steepening (usually inferiorly), increase in myopia and astigmatism with consequent loss of uncorrected as well as best corrected visual acuity,5 is a new area for CXL with promising early results.6,7 Other recent applications of CXL are in the treatment of bullous keratopathy3 and infective keratitis.8 As the efficacy of CXL is becoming more established and new applications for its usage are appearing, the number of patients seeking this treatment continues to grow. We see the standard protocol for CXL as moderately invasive as it requires mechanical removal of the epithelium; this has motivated us to develop a variant of the standard technique in which the epithelium is not removed, in order to offer patients a less invasive, safer and faster CXL while retaining the efficacy of the standard technique.
Materials and Methods
The cross-linking was carried out at the Zooprophylaxis Institute, Brescia, Italy, on four male albino rabbits (Oryctolagus cuniculus), approximately 60–90 days old, weighing 2–2.5kg. The rabbits were anaesthetised with intraperitoneal injection of xylazine and ketamine 15mg/kg.
Clinical treatment consisted of the standard reported CXL treatment,1 with the following variation: the anaesthetic drops used were benzalkonium chloride (BAK)-free, there was no epithelium removal and the riboflavin solution used contained 0.02% BAK (patented in Italy by Dr Roberto Pinelli) as a penetration enhancer. In each rabbit one eye was treated and the other eye served as a control.
A lethal dose of Tanax (Intervet, Munich, Germany), a solution used for painless death in pets and laboratory animals, was used to kill the rabbits. The procedure was performed in compliance with the Association for Research in Vision and Ophthalmology (ARVO)statement for the use of animals in ophthalmic and vision research, as well as Italian animal welfare law.
The eyes were then enucleated, rapidly washed in 0.1M phosphate buffer solution and immersed in 4% paraformaldehyde and 2.5% glutaraldehyde in 0.1M cacodylate buffered solution (pH 7.4) at 4°C (Sigma-Aldrich). After 30 minutes of fixation, the corneas were removed from each eye, sectioned into central and peripheral fragments and transferred into electron microscopy vials (EMS) containing fixative solution for four hours, during which time they were transferred to the Centro Interdipartimentale Microscopia Avanzata at the Università degli Studi di Milano. Fragments were then post-fixed in 1% osmium tetroxide, and gradually dehydrated in a series of ethanol solutions and finally in propylene oxide for 20 minutes. Infiltration was performed with propylene oxide–resin mixture (Araldite-Epon, Sigma-Aldrich) in a volume proportion of 1:2 for two hours, 1:1 overnight, 100% resin for four hours. Polymerisation was performed at 60°C for 48 hours. Sections were made on an Ultracut E microtome (Reichert, Austria); semithin sections (1.0–2.0μm) were stained with toluidine blue and photographed with a Leica DMRA2 light microscope (Leica, Germany). Ultra-thin sections of 80nm were collected on formvar/carbon copper grids of 200 mesh, double contrasted with uranyl acetate and lead citrate and examined at an EFTEM Leo912ab transmission electron microscope (TEM) (Zeiss, Germany) at 80kV. Digital images were acquired with an Esivision CCD-BM/1K system.
Results
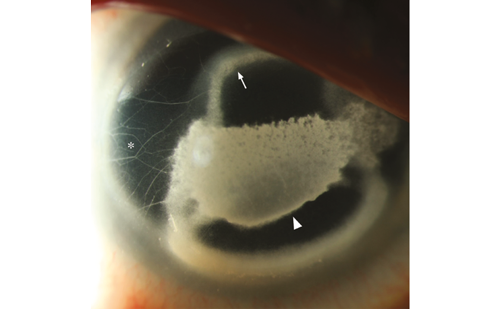
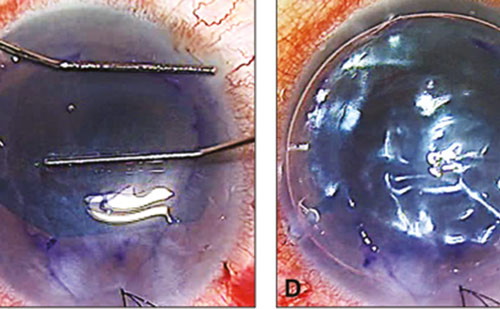
During the extraction of the corneas from the rabbit eyes, the treated corneas were noticeably stiffer and yellow in colour (see Figure 1), unlike the control corneas, which were flaccid.
Light Microscopy
Comparing the light microscope pictures of the treated and control eyes at 20x magnification, the following was noticed in the treated corneas in comparison with control corneas:
• the epithelial surface was straighter (retained curvature due to increased stiffness);
• the epithelium was more compact;
• in the stroma, the fibres showed more compact arrangement, and the fibres were straight compared with the wavy fibres in the stroma of the control corneas – this effect was noticed in approximately the upper 50% of the stroma; and
• the deep stroma adjacent to the endothelium looked the same as the control – the 40x images confirmed the same findings in the 20x× images (see Figure 2).
Electron Microscopy
Images of 16,000x magnification were obtained for the stroma. Sections from treated corneas showing the stromal fibres cut transversely at 90° from different layers of the stroma revealed the following on comparison with control corneas. • images from the upper 200μm of the stroma (see Figure 3) showed: • decreased inter-fibre distances, with more compact and regular arrangement of the fibres;
• increased number of fibres per unit area; and
• increased diameter of the fibres; and
• images from the lower 100μm of the stroma did not show any morphological differences between the control and treated corneas.
Discussion
The treated corneas on macroscopic examination showed increased stiffness in consistency. On microscopic examination this can be correlated with the straight collagen fibre arrangement in the upper 50% of the corneal thickness (which is about 200μm, as the average corneal thickness in rabbit eyes is 407±20μm).9 On TEM examination a far more regular collagen fibre arrangement, with reduced interfibre distances, was evident. From these results we concluded that CXL had occurred in this area. Further examination of the specimens at deeper stromal levels (bottom 100μm) did not reveal significant differences. The area between the aforementioned examined stroma in the treated corneas represented a transition zone where the regular fibre arrangement was not as obvious as in the upper 200μm of the cornea.
The benefit of CXL treatment for patients with progressive KC is undoubted, and in the near future it could become the gold standard for other conditions such as post-LASIK ectasia. The standard procedure for performing the CXL treatment requires epithelium removal. The reason for this step is that the epithelium and its tight junctions act as a barrier against the diffusion of the riboflavin solution into the stroma. However, this step is responsible for most of the complications reported to date with the CXL procedure.
The most obvious and unavoidable complication is the discomfort and pain the patient experiences until full re-epithelialisation of the cornea occurs. Whatever the mechanism of removing the epithelium (mechanical, alcohol-assisted or by excimer laser ablation), this complication is unavoidable.10 Most surgeons performing standard CXL mechanically remove the epithelium; this can leave a rough stromal bed that may impede epithelial healing. It was noted that with mechanical removal there are Bowman’s layer defects, an irregular anterior stromal surface and retained islands.11 It is estimated that re-epithelialisation requires at least four days to complete and up to three months for qualitative improvement of the epithelial cell mosaic compared with the pre-operative state by confocal microscopy.12 In the period of re-epithelialisation there is an accompanying stromal oedema.1
The second consequence of mechanical debridement is the destruction of the intra-epithelial and sub-basal nerve fibres in an area wider than the treatment area, as well as the aggravation of the destruction of centrally located nerve fibres up to the anterior stroma by the combined effect of mechanical debridement and riboflavin–UVA exposure. Regeneration requires six months to complete.13
Other occasional reported complications include:
• activation of herpetic keratitis, where the use of corticosteroids along with the epithelial debridement and corneal nerve damage may have contributed to this activation;14 and
• induction of diffuse lamellar keratitis (DLK) in post-LASIK patients, as epithelium removal is suggested to release cytokines, which starts the cascade that brings about DLK.15
Along with the aforementioned complications, the time needed to remove the epithelium is added to the already lengthy (30 minutes) UVA exposure time under topical anaesthesia. To avoid epithelium removal and hence the complications and limitations, while at thesame time retaining the efficacy of CXL treatment, would surely make it a much less invasive procedure.
Some authors have reported the use of femtosecond laser to create a sub-epithelial pocket for intrastromal delivery of riboflavin.3 This approach is good in the sense that it avoids epithelium removal; however, it requires the use of an expensive,non-portable femtosecond laser machine, which is not available at all centres providing CXL and is not feasible to acquire only for this use.
Our results demonstrate signs of corneal cross-linking without removing the epithelium, by the use of BAK as a tensioactive substance. A tensioactive material, a surfactant or an active surface agent is a chemical substance that changes the surface tension value. BAK is one of the most popular preservatives used in ophthalmic drops, present in about 72% of eye drops with a concentration range of 0.004–0.02%.16 Along with its antimicrobial properties it is a tensioactive chemical that rapidly increases corneal permeability due to the disintegration of the tight junctions and the hanges in the cell membranes of the superficial epithelial cells.17 At he concentration used in commonly available eyedrops and in the solution used in this experiment, it can cause lifting and peeling of some superficial epithelial cells with exposure of the second layer of cells (wing cells), with no change in the basal epithelial cells or the endothelial cells.17–19 These are the immediate side effects of BAK, whereas other side effects from chronic exposure are not relevant to this experiment. The estimated half-life for BAK elimination from the corneal tissue is 20 hours.20
This first ever published, preliminary study demonstrated that CXL can take place without removing the corneal epithelium. However, this should be confirmed and supported by further investigations such as stress–strain measurements, resistance to digestive enzymes, thermo-mechanical and hydration behaviours of the cross-linked corneas with this technique, as well as comparing it with the standard CXL technique. Also, investigations to demonstrate the safety of the procedure on endothelial cells should be carried out, although the effect of cross-linking was observed far from the endothelium. In conclusion, the use of BAK with riboflavin may overcome the need for corneal epithelial removal to carry out CXL, and hence offer a less invasive procedure with many fewer complications.