Ocular trauma is an important worldwide cause of preventable morbidity and accounts for half a million cases of monocular blindness worldwide.1–5 Paucity of epidemiological data regarding ocular trauma in the developing world is a major factor in implementing effective health policy measures.
The only national estimate regarding the Indian subcontinent is from a survey conducted from 1971–1974, where ocular trauma accounted for 1.2% of national blindness.6 An ideal data collection system for ocular injury should incorporate population-based comparisons using a known denominator; demographic data, details of injury, visual acuity (VA) at presentation and final outcome after appropriate management.7 Factors that have been found to correlate significantly with visual outcome post ocular trauma include age,8 type or mechanism of injury,2,9–13 initial VA,2,11–13 presence of relative afferent pupillary defect (RAPD),8,11–14 extent of wound and size of open globe injury,2,11–13 location of open globe wound,2,10–13 lens damage,2,11–13 hyphema,11,13,15 vitreous hemorrhage,2,11,13,15–16 retinal detachment,17 and presence and type of intraocular foreign body (IOFB).18 This study was conducted keeping these parameters in mind and assessing the requisite denominators.
Materials and methods This study was a prospective observational study of all patients admitted to a tertiary hospital with ocular trauma between December 2012 and March 2014.
Inclusion/exclusion criteria Since this was an epidemiological study, all patients irrespective of their age, mode of injury, time since injury, presenting VA, reporting to the emergency services of the hospital were included in the study after the requisite consent to be a part of the study and willingness for follow up.
Data collected were demographic profile, type and mode of injury, first aid received, complete ophthalmic evaluation including appropriate investigations (X-ray Orbit, Ultrasonography, computed tomography [CT] scan wherever applicable). All patients were graded from A–E based on presenting VA as per Birmingham Eye Trauma Terminology (BETT).19 The zone of injury was graded from II–III for open as well as closed globe injuries. Ocular Trauma Scoring System (OTSS) was computed to
assess the prognosis of final visual outcome of the patient.20 All patients with vision equal to or worse than grade D, zone II and III injuries, hyphema on initial presentation, subluxated lens, RAPD, IOFB, vitreous hemorrhage, retinal detachment, and endophthalmitis at presentation were classified as “severe” injuries. For injuries with multiple diagnoses, those with a “severe” component were categorized as severe.4
All patients were managed as per standard management protocol, whether surgical or medical, followed by appropriate medical management. Ultrasound was conducted after 48 hours of surgical intervention whenever preoperative ultrasound had not been performed. This was to confirm or exclude posterior segment involvement. Secondary intervention like cataract extraction, IOFB removal and retinal detachment surgery were planned and performed at appropriate time intervals.
All patients were followed up for 6 months and evaluated for VA (near and distance), inflammation (anterior segment or retrolental) in both the injured and non-injured eyes. The latter was done, keeping in mind the propensity of sympathetic ophthalmitis and assess requirement of any further intervention in both the injured and normal eye. All patients received two broad-spectrum systemic antibiotics for at least 7 days, two topical fortified antibiotics (vancomycin plus ceftazidime or cephazolin plus tobramycin) for at least 6 weeks after the injury. Oral steroids were administered in cases with potential risk of sympathetic ophthalmitis (ciliary body injury, mutilating iris trauma, non-infected perforations). VA ≥6/60 was defined as “good” vision post intervention (Grade A and B).
All the procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional or regional) and with the Helsinki Declaration of 1975, revised in 2000.
All the data collected were analyzed using SPSS version 17.0 software. Routine statistics, including means, proportions and Chi-square tests were carried out. Odds ratio (OR) and 95% confidence intervals (CI) were computed to evaluate the strength of association between various factors.
Results A total of 103 patients were evaluated for the duration of study over a period of 15 months. All patients were followed up for a minimum of 6 months.
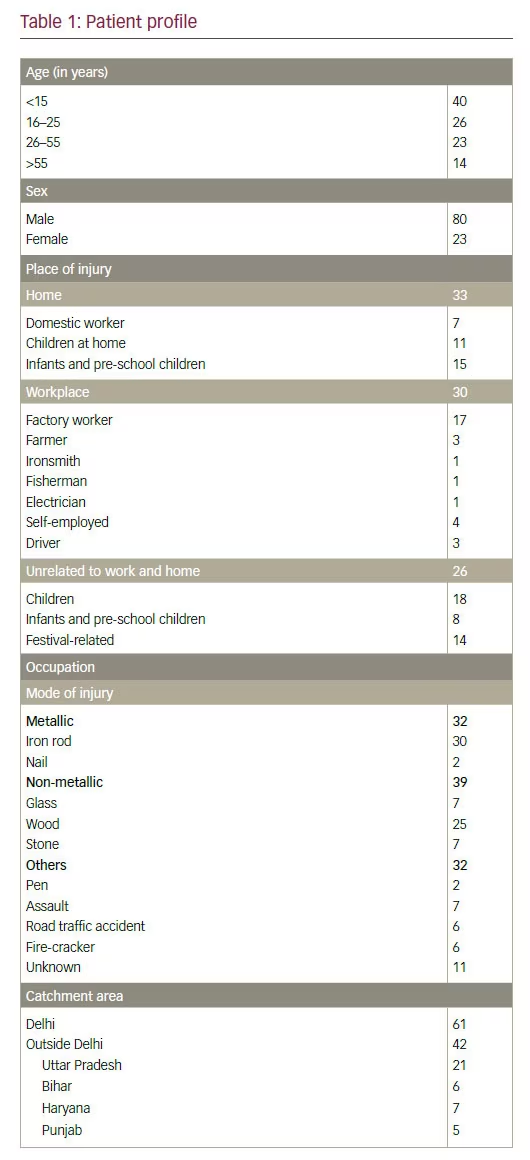
Demographics Most patients (64%) were younger than 25 years of age and most injuries (71%) were unrelated to work or the patient’s occupation (see Table 1).
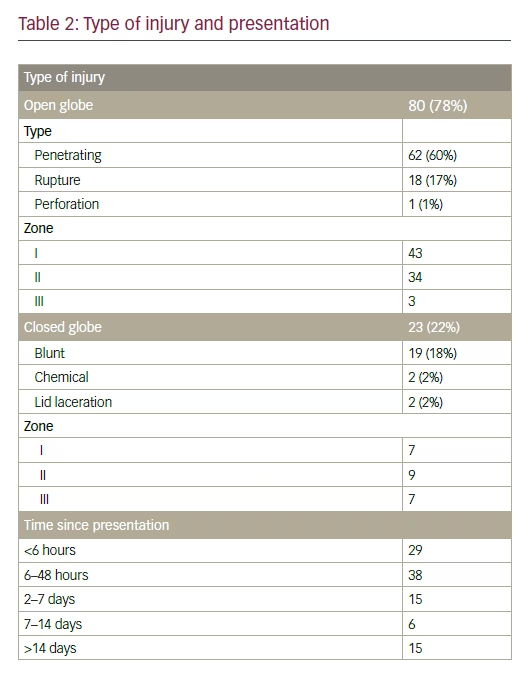
Initial clinical presentation Seventy-six patients had poor VA of Grade D or E on initial presentation. The proportion of open globe to closed globe injury was 78:22; 77.5% open globe injuries being penetrating. Seventeen patients had globe rupture and one patient had globe perforation. Injury grade was zone I in 43 patients, zone II and III injuries in 34 and three patients, respectively (see Table 2). In 23 patients with closed globe injury, nine had injuries confined to zone I, seven each to zone II and zone III. The mean OTSS score was 46.27.
Imaging (X-ray orbit) revealed intra-ocular foreign body in nine (8.7%) cases, or 11% of all open globe injuries. In the entire series, 82 (80%) patients were categorized as having “severe” ocular trauma.
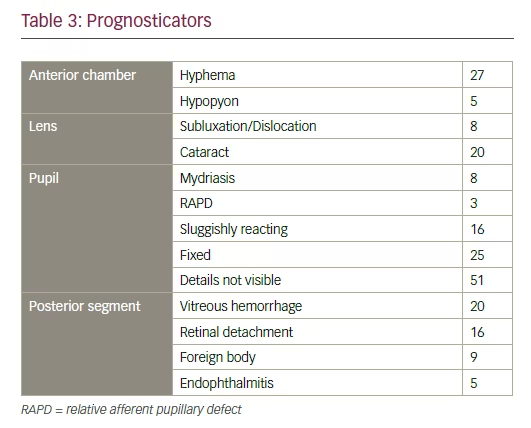
Ultrasonography performed either at presentation or 48 hours after initial repair for posterior segment evaluation documented vitreous hemorrhage and retinal detachment in 20 and 16 patients respectively. Endophthalmitis occurred in five cases of penetrating trauma out of 103 patients (5%). Ninetytwo cases (89%) had some form of anterior segment trauma whereas 60 patients (58%) had posterior segment trauma singly or in combination with anterior segment injuries. (see Table 3)
Follow-up All patients were followed up for a minimum period of 6 months. VA at the end of 6 months was recorded and graded from A to E as per grading of presenting VA (see Figure 1).
Good visual outcome was attained in 52 cases (50.4%), of which 48 patients had anterior segment injury and 12 had either posterior segment injury alone or along with anterior segment injury. In the subgroup of patients with
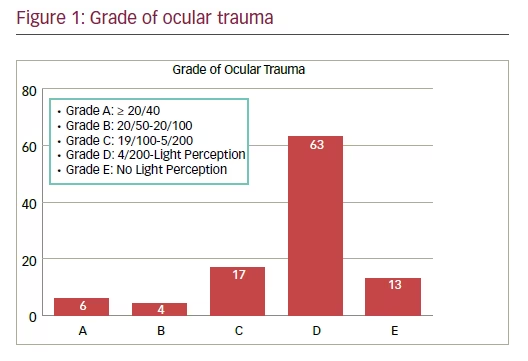
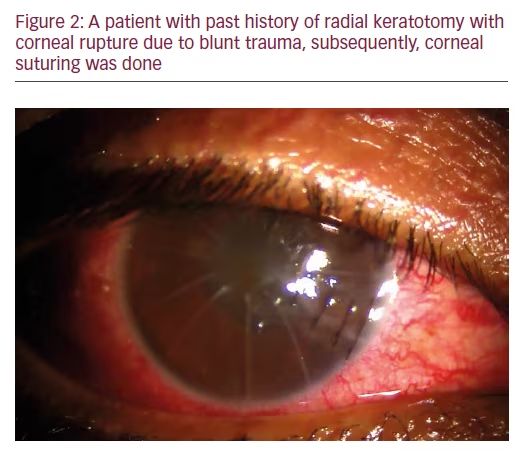
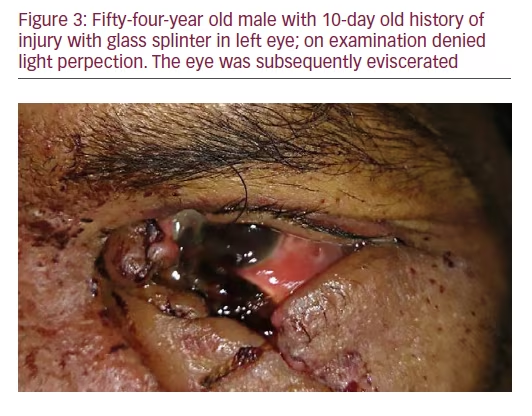
good visual outcome, 56% presented within 48 hours of injury. In those with poor outcome (final vision <6/60), late presentation beyond 48 hours was seen in 41.2% cases (see Table 4).
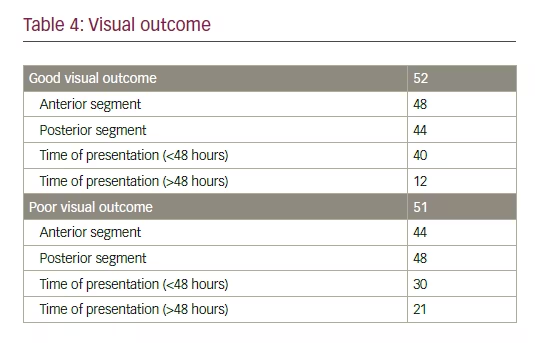
Discussion This prospective, hospital-based study provides data on the current pattern of serious ocular injuries in patients admitted to a tertiary care center in the emergency department.
Most of the patients who sought healthcare for ocular trauma were males (78%). This could be explained by the health-seeking behavior of the population studied, where males are given preferential treatment. Previous studies have highlighted this aspect citing increased vulnerability of male gender in being exposed to outdoor work activities in agriculture and industry10–11,19–22 However, this does not particularly hold true for our study, where home-related injuries predominated.
Children and young adults were commonest age group to be afflicted, because of their adventurous activities and treatment being sought more often, compared with the neglected elderly population. Studies from both developed and developing worlds have confirmed this aspect of ocular trauma.1–3,5,25 The restricted mobility of the elderly leading to inability in accessing medical facilities situated at distances could be another reason for this disproportionate statistic. A significant proportion of patients (42 of 103) had travelled from neighboring states to avail themselves of adequate and economically viable treatment facilities. This reflects the large catchment area and inadequate access to tertiary hospitals providing subsidized treatments. The high proportion of “serious” ocular trauma observed in this study at 80% could be due to weeding out of less serious cases treated at peripheral healthcare facilities.
The study revealed that the most injuries occurred at home and lack of basic safety precautions was the common factor. This is at variance with previous studies reporting work related injuries to be more common.4,26–30 These findings have implications for health and safety strategies in prevention of serious eye injuries. The current emphasis on safe work environments must be expanded to include the home environment. Inculcating awareness of hazardous activities involving domestic tools and use of specific protective eye wear needs to be highlighted. It is likely that the magnitude of domestic ocular injuries is even greater and that the reported cases are just the tip of the iceberg.
A significant number of injuries (13%) were festival-related, for example through bow-and-arrow-related injuries or fire-cracker-related injury during Dussehra and Diwali, festivals indigenous to our country. As most of these injuries occurred in children, it underscores a lack of awareness among parents about the hazards of leaving children unattended during these popular festivals. Many countries have used legislative measures to regulate the use of fireworks.31–32 Implementation of similar legislative measures would go a long way in reducing firework-related injuries in India. Apart from these regulations, legislation should stipulate all safety measures including the age limit for independently handling these devices, as well as the minimum distance that ought to be maintained while lighting firecrackers and watching fireworks. Children should handle firecrackers only under adult supervision and use protective eyewear while handling the firecrackers.33
The reporting time of the majority (68%) of patients was within 48 hours of injury, highlighting increased awareness among people to seek early medical intervention for ocular trauma. This reflects success of mass awareness campaigns initiated for preventing avoidable blindness.
Good visual outcome (final best corrected VA ≥6/60), could be attained in 52 cases, of which 53% had anterior segment injury alone and 20% had concomitant retinal injury. Chi-square values without Yates correction equaled 15.73 with one degree of freedom and two-tailed p-value <0.0001, make the association between anterior segment injury and visual outcome extremely significant. Patients with posterior segment injury, particularly those with intra-ocular foreign body (11% of all open globe injuries) had more adverse visual outcome in view of increased incidence of vitreous hemorrhage, retinal detachment and endophthalmitis associated with it. (see Table 3). The cutoff of 6/60 was taken, keeping in mind the definition of blindness to be <6/60 as per Indian National Programme for Control of Blindness (NPCB) guidelines.34
A determinant for good visual outcome was early presentation within 48 hours of injury; 57% patients with early presentation had good visual outcome (see Table 4). Conversely, poor outcome was associated with late presentation beyond 48 hours; seen in 64% cases with late presentation. Statistical test of Chi-square without Yates correction, equaled 3.87 with one degree of freedom found two-tailed p-value to be 0.049, implying statistically significant correlation between early presentation and better visual prognosis. The statistical significance was, however, diluted due to confounders like early endophthalmitis and auto-evisceration, which had nil visual prognoses.
Ocular trauma in developing countries has not been studied extensively. This study in a developing country such as India underscores that trauma remains a significant cause of monocular vision loss in all age groups with a large proportion affecting younger patients, thereby entailing increased lifetime of disability years. The need for adoption of safe behavior in the home environment, which is traditionally envisaged as safe, use of protective eyewear to avoid most workplace-related injuries and early intervention are other aspects highlighted by this study.







