Delivery of bevacizumab via anterior segment route in pseudophakic eyes is a safe and effective method for treatment of ARMD degeneration and DME that minimizes the possibility of injury to the retina or sclera.
In 2006, the US Food and Drug Administration (FDA) approved Genentech’s ranibizumab (Lucentis®), a Fab fragment of a humanized monoclonal anti-vascular endothelial growth factor (VEGF)-A designed for intraocular use for the treatment of exudative age-related macular degeneration (ARMD). Since 2006, ranibizumab and its parent monoclonal antibody bevacizumab have been extensively used to treat exudative ARMD. Intravitreal injections of bevacizumab and ranibizumab have become the most common treatment for exudative ARMD resulting in visual stabilization in 90 % of patients and a gain of 3 or more lines of visual acuity (VA) in 30–40 % of the patients.1–3 Even though the development of inhibitors of VEGF has transformed the treatment of exudative ARMD and other ocular neovascular
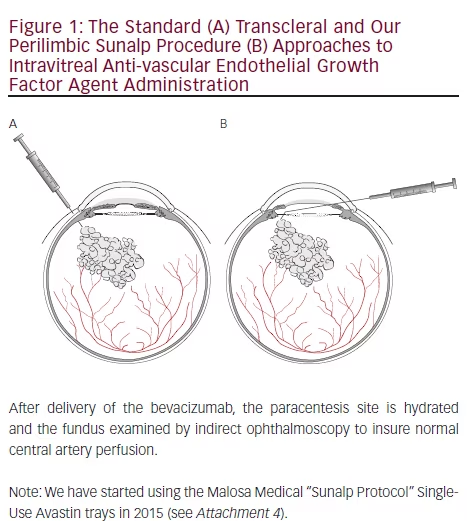
diseases, the repeated intravitreal injections necessary to prevent the reoccurrence of neovascularization are not without side effects. These include endophthalmitis,4 ocular hypertension, submacular hemorrhage, and the possibility of systemic diffusion resulting in long-term thromboembolic events.5–8 Since the introduction of the anti-VEGF antibodies bevacizumab (Avastin®) and ranibizumab (Lucentis) for the treatment of ARMD, ophthalmologists have used these anti-VEGF for the treatment of other neovascular ocular diseases, such as proliferative diabetic retinopathy, diabetic macular edema (DME), and cystoid macular edema (CME).8–11 Even though the rates of serious ocular adverse events are low, in the range of 1–2 %,8,9 the increased use of these drugs has meant an number of cases with significant serious side effects. Intravitreal injection with an anti-angiogenic drug is accomplished by anesthetizing the patient locally with an injection of lidocaine or a topical anesthetic, followed by the injection of the anti-VEGF, usually infero-temporally, 3.5 to 4 mm posterior to the limbus through the pars plana. Even though the procedure is simple, it is not possible to observe the precise site where the injected agent is delivered, thus risking possible injury to the retina and choroid and lens. In addition, the injection in painful and frightening for the patient (see Figure 1A). To decrease the difficulties associated with intravitreal injections we have explored the delivery of bevacizumab via a corneal route in pseudophakic eyes. Here we report that the delivery of bevacizumab via a corneal route is effective in decreasing edema in patients with diabetes and in stabilizing and/or increasing vision in exudative ARMD patients, while minimizing potential retinal damage and adverse affects on corneal endothelial cells (see Figure 1B).
Material and Methods
Administration Procedure
Informed consent was obtained from all patients.
The eye is dilated using one drop of tropicamide ophthalmic solution (1 %) and one drop of phenylephrine hydrochloride ophthalmic solution (2.5 %). The patient is placed supine under the operating microscope with the microscope light off. After scrubbing the eyelids with 1 % povidone iodine, a drop of povidone iodine is instilled in the eye, followed by a drop of the local anesthetic, 0.5 % tetracaine hydrochloride (Alcon Laboratories, Dallas, TX, US). The eye is draped with Tegaderm dressing (3M, St Paul, MN, US). A lid speculum is placed.
A Mastel ring light and fixation light are used to fixate the eye. Using an Alcon (Fort Worth, TX, US) single-use ophthalmic 15° angled knife, a 0.4 mm paracentesis is made at the limbus at 11 o’clock.
A 27-gauge irrigating, 5 mm angled cannula, attached to a 1.0 ml syringe is fitted into the paracentesis incision and advanced through the limbus and through the anterior and posterior chamber. The cannula is maneuvered through the zonules into the vitreous, the tip of the cannula and bevacizumab release can be visualized within the vitreous. Bevacizumab (0.1 ml) is injected into the vitreous cavity (see Figure 1B), and the cannula is removed immediately so as not to chafe the iris. Betadine and antibiotic drops are placed.
Patients
Avastin was administered via the corneal route in (a) nine eyes with neovascular ARMD from five patients ranging from 74 years to 92 years of age; (b) in 38 eyes from 21 diabetic retinopathy patients ranging in age from 47 to 80 years of age; (c) two eyes from two CME, aged 68 and 80, respectively; and (d) one eye from a central retinal vein occlusion (CRVO) patient 65 years of age.
Visual Acuity
VA was measured pre-injection and at 1 day post-Avastin administration in all eyes and at 1 month post-Avastin administration in 16 eyes.
The average pre-injection VA in the eyes of ARMD patients was 20/250 and after 1 day the average was 20/150; three out of nine eyes gained 3 or more lines, five remained stable and one deteriorated. In 16 eyes from 12 patients who returned for an examination at 1 month pre-injection VA was 20/70 and post-injection VA was 20/50. The average pre-injection VA in patients with diabetic retinopathy was 20/150; 11 eyes gained 2 or more lines, seven eyes gained 3 or more lines; in 36 eyes vision remained stable and in only one eye vision deteriorated. No significant change was observed in the two eyes from the CME patients. Some patients were lost to follow up.
Macular Edema
Macular edema was determined using the Heidelberg and NIDEK units (see section on Optical Coherence Tomography Equipment), 50 eyes of 29 patients, which included 21 DME patients, five ARMD patients, two CME patients, and one CRVO patient. Macular edema was significantly lower 1 day and 1 month after Avastin administrations as shown by the Wilcoxon rank-sum test (p=0.00358) and confirmed with the optical coherence tomography (OCT) pictures. Representative OCTs from DME (see Attachment 1), ARMD (see Attachment 2), and CME (see Attachment 3) patients all show that after one injection the edema has decreased.
Optical Coherence Tomography Equipment
1) Heidelberg OCT (Heidelberg Engineering GmbH, Heidelberg, Germany).
2) Nidek OCT RS-3000 Advance (NIDEK Co., Ltd, Hiroishi, Japan).
Corneal Endothelial Cell Counts
Using a Konan specular microscope corneal endothelial cell counts and morphology were performed on 43 eyes from 24 patients. Statistical analysis of endothelial cell counts was carried out using a paired t-test.
No significant changes in corneal endothelial cell morphology and counts were observed one day after Avastin administration. The pre- Avastin endothelial average cell counts for the 43 eyes were 2,580.47 ± 192.88 and the post-Avastin counts were 2,490.05 ± 232.94; p=0.0442. The difference between pre- and post-Avastin administration is not significantly different.
Discussion
With the approval of ranibizumab (Lucentis) in 2006 and the off-label use of bevacizumab (Avastin) ophthalmologists are treating neovascular macular degeneration and other retinal neovascular diseases, intravitreal injections have become routine in practices specializing in retinal diseases and in many general ophthalmology practices. Even though the rate of adverse side effects is low8,9 the number of intravitreal injection is so large that even these low rates result in significant numbers of patients suffering adverse events. In 2008, the number of intravitreal injections billed to Medicare was over one million in the US12 and it may now have reached three million; with three million intravitreal injections at the rate of 2 % adverse events would affect 60,000 patients in the US alone.
Some complications associated with intravitreal injections, such as conjunctival hemorrhage, retinal tears, and retinal detachment are caused by the injection through the sclera without the ability to visualize the delivery point. We have shown that it is feasible to administer Avastin via a corneal route in the vitreous cavity in pseudophakic patients without any complications and with similar effectiveness as administration via the intravitreal route, and with minimal discomfort and no pain.
Is the administration of Avastin via the corneal route safe and is there is loss of drug via aqueous outflow? A number of studies in animal models and in humans13–15 have shown that intracameral bevacizumab for the treatment of neovascular glaucoma in humans is safe and effective and does not have any harmful effects on the cornea and on endothelial cells in particular. Our data support other findings that injections of bevacizumab via the corneal route does not affect endothelial cell numbers or morphology.
To our knowledge, there are no studies on the effect of corneal route administration of anti-VEGFs on choroidal neovascularization (CNV). However, there are a number of studies in animals that show that intravitreal injection of bevacizumab diffuses freely into the aqueous and cornea. In a study on the effect of bevacizumab on corneal neovascularization in animal models both intracameral and intravitreal administration were effective and bevacizumab was detected in the anterior chamber by day 2 after administration.16 In a similar study, ranibizumab was detected in the aqueous 3 days after intravitreal injection17 indicating that these drugs persist in the vitreous and aqueous for some time. In fact, half-life of ranibizumab in the vitreous is 2.88 days and the half-life in the aqueous is 2.84 days17 indicating that these drugs do not exit with aqueous flow.
Since the route of penetration into the posterior retina of bevacizumab or ranibizumab is not known nor is known what the effective concentration of either of these drugs is necessary to inhibit CNV, the only reliable means to assess effectiveness is by experimentation. In the present study, VA improved in three of the nine eyes of neovascular ARMD patients, was stabilized in five eyes, and deteriorated in one; this result is similar to results obtained in a number of large studies using intravitreal administration. In addition, OCT images in our study clearly show that the edema accompanying diabetic retinopathy, exudative ARMD, and cystoid macular edema did recede following administration of bevacizumab via the corneal route indicating that an effective concentration of the drug reached the subretinal space. To our knowledge this is the first study demonstrating that corneal route administration of bevacizumab is effective for the treatment of subretinal neovascularization.
Summary Statement: Delivery of bevacizumab via anterior segment route in pseudophakic eyes is a safe and effective method for treatment of ARMD degeneration and DME that minimizes the possibility of injury to the retina or sclera.







