“Look… Up in the sky… It’s a bird… It’s a plane… No, it’s supertechnology.” Commonly performed in Europe, South Africa, Canada, and China, corneal collagen cross-linking (CXL) is still off-label in the US. Why? Despite the proven effectiveness and safety of the procedure in many countries around the world, many feel that the lack of approval in the US is because of US Food and Drug Administration (FDA) bureaucracy and suppression of innovation.
Clinical Perspective
Developed in response to the need for a treatment for the ectasia of ketatoconus, Seiler et al., in the 1990s, introduced a procedure that was a fusion of vitamin therapy with corneal epithelial surgery.1 The procedure has been shown to virtually stop the advancement of ectasia in keratoconus and that following excimer laser ablation. In their reported series, the biomechanical status of the cornea was stabilized, with minimal side effects and few complications.
Cross-linking of collagen refers to the capacity of collagen fibers to form strong chemical bonds with adjacent fibrils. Some cross-linking naturally occurs in the cornea with aging, but for therapeutic effect underprecise control, chemical agents (ultraviolet [UV]-activated riboflavin [RF]) are used.
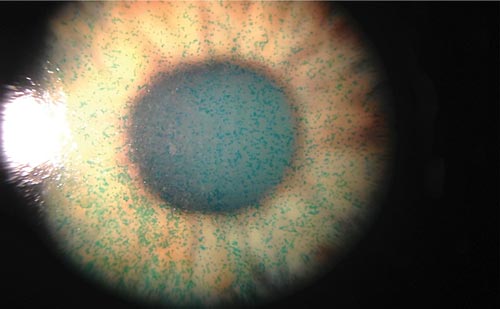
In addition to the progressive degenerative condition keratoconus, corneal ectasia can occur following any type of corneal surgery, such as laser-assisted in situ keratomileusis (LASIK) procedures and radial keratotomy (RK), and in pathologic peripheral degeneration (marginal corneal dystrophy) (see Figure 1).
Femtosecond Laser for Corneal Eye Surgery
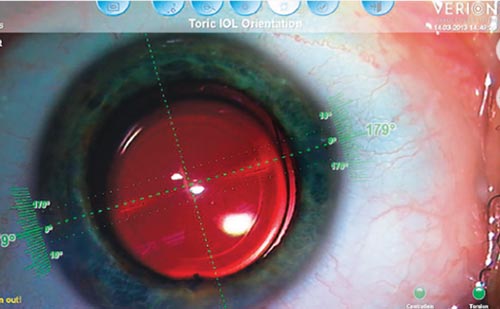
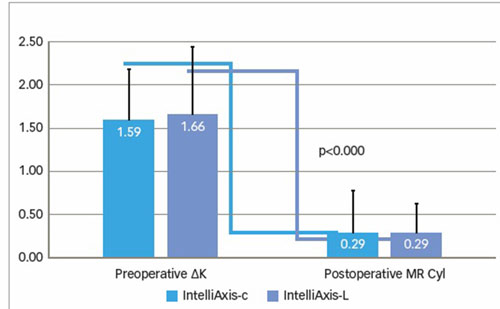
While there is no doubt that the microkeratome is a great tool for surgeons performing laser eye surgery, the femtosecond laser appears to be more accurate. But complications (transient light sensitivity, irregular flap with induced astigmatism, and ectasias) still occur. Dry eye syndrome is also a problem. The search for effective treatment continues (see Figures 2 and 3).
Progressive irregular corneal thinning is problematic with any LASIK procedure. Developed as a method of strengthening weakened corneas of keratoconus, CXL has been shown to strengthen the corneas in post-LASIK ectasias and in marginal corneal dystrophies.2
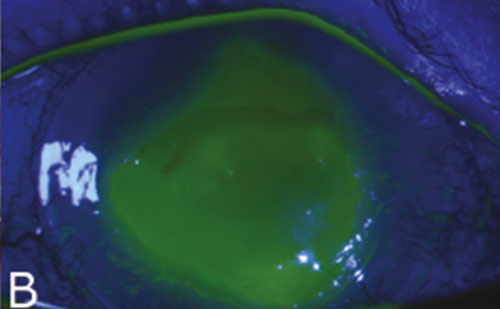
Immunofluorescent confocal microscopy has shown a pronounced compacting of collagen fibers in the anterior stroma after RF and UVA exposure (see Figures 4–5). How it works. The photosensitizer RF and UV irradiance lead to corneal tissue strengthening by increasing collagen covalent bonds, as in photopolymerization in polymers. The cross-linking leads to a significant increase in collagen fiber diameter.
Method
The cornea is saturated with RF, then illuminated with UVA at a frequency of 365 nm, a wavelength that is strongly absorbed by the RF. The RF has a dual action of producing free radicals that cause cross-linking of the stromal collagen, creating new, stable bridges between collagen molecules, reinforcing the corneal structure, strengthening the cornea, and acting as a shield to prevent significant levels of UV from penetrating deeper into the eye (see Figure 7).Cases of irregular astigmatism caused by ectasia have been treated by initial cross-linking followed by custom topography-guided surface ablation, with restoration of vision and stabilization of the ectasia and improvement of patients’ visual, refractive, and topography outcomes.3,4
John Marshall has demonstrated that by increasing the power the effect can be the same in less time. He states, “We can play around with the power-time complex to deliver the same amount of energy to the cornea in less time” (see Figures 8–10).5
Validation
Leading experts have stated, in examining the data over the past 10 years, “If cross linking had been available in the United States as it was in other parts of the world, 50 % of the corneal transplants could have been avoided.” (Doyle Stulting, personal communication, April 2013.) It is apparent that if CXL had been readily available in the 1980s, RK could still be the procedure of choice for myopia and astigmatism today.
No medical or surgical procedure is perfect or complication free, but complications of CXL appear to be infrequent and manageable.Severe pain and visual loss may remain until epithelial regrowth occurs. Stromal haze, present during the first few weeks, usually resolves within 3 to 6 months.
Several pioneers of cross-linking have reported, “The almost complete absence of adverse reactions to the treatment has been confirmed by several studies. The failure rate in my series is less than 3 % and the complication rate is less than 1 %.” (Theo Seiler, personal communicaton, January 2012.) Joseph Colin wrote, “We remove the epithelium for better efficacy. However, investigators are now producing a new riboflavin preparation with modified physiochemical properties that will be able to penetrate the cornea through the epithelium.”6
Roberto Pinelli reports, “The epithelium does not significantly restrict the riboflavin penetration. In our series, RF 0.1 % was applied to the cornea via a saturated Merocel sponge for five minutes before the start of UVA light administration, and reapplied every three minutes during the whole procedure. At six and nine months post-op there was no significant difference in the analyzed parameters between the depithelialized group and the non-depithelialized one.” (Personal communication, June 2012.)
Transepithelial CXL appears to be a major advance. RF is a hydrophilic compound and cannot easily cross the intact epithelial barrier. Buffers and ethylenediaminetetraacetic acid (EDTA) ‘enhancers’ are added to RF solution to help penetrate through intact epithelium.7,8 The addition of pulsed illumination with added oxygen has increased effectiveness in some studies (see Figure 11). (Francis Price, personal communication, July 2013.)
Conclusion
With continued refinement and improvement of technique, RF/UVA CXL may become the treatment of choice in stabilizing thinning or unstable corneas. FDA roadblocks should be reduced by shared information of an informed medical community. As additional applications and improved methodology are developed by investigators, transepithelial methodology will improve and become standard, and CXL will take its place as a method of choice in the treatment of ectasias of all etiologies.