The principles of wavefront optics from optical engineering have been adapted for use in measuring irregularities in the refractive power of the eye. These variations, which occur over the entrance pupil, are collectively called aberrations and are measured with a wavefront sensor. Wavefront technology applied to ophthalmology represents a paradigm shift in the way optical aberrations can be measured, described, and treated. In addition to considerable utility as a diagnostic tool, wavefront technology combined with a femtosecond laser has the potential for correcting visual deficits beyond sphere and cylinder. The goal of wavefront-guided (WFG) laser-assisted in situ keratomileusis (LASIK) is a more optically perfect ablation based on all of the optical aberrations measured with a wavefront aberrometer.
Preoperative Diagnostics
WFG LASIK, also called custom LASIK, is a variation of refractive surgery where, in the preoperative stages, a highly precise road map of the eye is generated, detailing all higher and lower order aberrations (HOAs/LOAs) in the eye.1 This wavefront capture is the salient element that directly relates to the quality of the laser ablation. An accurate assessment of the aberrations of the eye allows the surgeon to tailor the excimer laser, and, rather than applying a sphero-cylindrical correction to the cornea, the laser is instructed to ablate a sophisticated spatially variant pattern based on measurements from an aberrometer. Major factors that contribute to achieving optimal ablation outcomes include appropriate patient selection, high-quality wavefront data, successful surgery, and accurately predicting and managing the changes that occur during healing.2
Wavefront Sensing Methods and Devices
Wavefront measuring systems in the optical industry are primarily based on one of the following principles: Hartmann-Shack, Tschering, raytracing, or refractometry. Most optical wavefront sensing devices that are used in conjunction with an excimer laser employ a Hartmann-Shack sensor. In this device, light exiting the eye is divided into a grid pattern for analysis by a lenslet array providing views from different angles within the pupil. Aberrations can be calculated by measuring the distance and angle of each spot from its expected position in an ideal eye.
In the Tschering method, a known pattern is projected onto the retina and the resulting distortions in its shape are related to the aberrations of the eye. The ray-tracing system can be included in this category of wavefront sensor, with a difference in the type of pattern projected. The last method, refractometry, relies on subjective patient response. Dynamic skiascopy is used to measure the refraction of the eye, through the pupil, of over 1,440 points. It provides the nearly simultaneous measurement of wavefront and corneal topography.3
Wavefront Capture
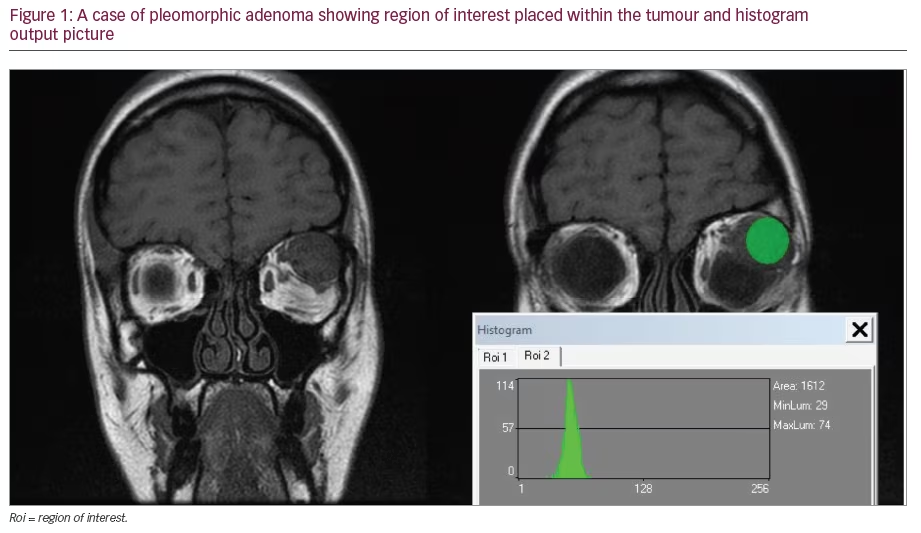
The precision of laser ablation depends on obtaining an accurate assessment of the aberrations of the eye. The quality of each capture needs to be monitored by assessing the lenslet pattern and drop-out points. Transient drop-out that varies between captures usually indicates a dry spot on the cornea, whereas an area of consistent drop-out can indicate an opacity in the optical system (see Figure 1). The captures should be repeated as needed to obtain high-quality images. The variability in the derived defocus (sphere) between captures is a useful tool to ensure accurate measurements. The size of the wavefront (cross-sectional area) is determined by the size of the entrance pupil. Therefore, the wavefront unit should be located in a dim room to allow a large pupil capture, with a pupil size of 5 mm as the generally accepted size. Some physicians utilize low-strength tropicamide to increase the pupil size for the aberrometer capture, although there is some concern about the potential shift in the pupil centroid.
Manufacturers have designed their wavefront units to minimize the tendency for a patient to accommodate (instrument myopia). Despite this, accommodation during a capture is always a concern and needs to be monitored and minimized in those laser systems that base their capture on a natural pupil. Checking the difference between the manifest sphere and the wavefront-derived sphere is imperative. Careful patient instruction, such as not allowing them to read just beforehand and telling them to look beyond the instrument during the capture can help. Some laser systems rely on a cycloplegic capture, which allows for a large pupil capture without accommodation concern.
Lower Order Aberrations
The order of aberrations refers to the complexity of the shape of the wavefront emerging through the pupil. LOAs consist of conventional spherical and cylindrical refractive errors that represent approximately 85 % of all aberrations in an eye. Correcting LOAs has the highest impact on unaided acuity, which is the eye’s ability to distinguish object details and shape. LOAs can generally be corrected with a spectacle or contact lens, although many patients choose LASIK to be free of their corrective lenses. Wavefront technology measures all of the aberrations of the eye. This can be conceptualized by considering a light source emanating from the macula and going back out of the eye. The light rays get refracted as they pass through the lens and cornea. Retinoscopy relies on the same principle. A wavefront is then constructed by forming a surface using the ends of the exiting light rays. The X-Y dimensions of the wavefront would be the same as the entrance pupil. The Z dimension is representative of the aberration of the eye, also called the optical path deviation. An emmetropic eye without any LOAs or HOAs would have parallel rays exiting the eye and hence a flat wavefront. If the eye is myopic, exiting light rays converge so the wavefront would be concave. If the eye is hyperopic, the light rays diverge, so the wavefront would be convex. Astigmatism would be represented by a saddle-shaped wavefront.
Higher Order Aberrations
More complex aberrations include distortions such as coma, trefoil, and spherical aberration, as well as numerous others that cannot be adequately corrected through spectacle lenses. These more complex aberrations are now collectively called HOAs and can be represented in the system described above by a more complex wavefront (see Figure 2). The shape of the wavefront, which describes the total aberration of the eye, can be mathematically described by using a series of Zernike polynomials, named after the mathematician Frits Zernike. With the Zernike method, names have been established for specific aberrations including defocus, cylinder, prism, coma, trefoil, and others, allowing the clinician to describe and understand the etiology of visual compromise.
HOAs are taking on clinical relevance as more is known about how they affect vision. The total amount of HOAs can be incorporated into a single number by computing the root mean square (RMS) of the wavefront deviation after the sphere and cylinder components have been mathematically removed.
One limitation to the Zernike method is that aberrations of the eye are mathematically ‘fit’ into the individual terms. LOAs (sphere and cylinder) and some HOAs (coma and spherical aberration) match well with Zernike terms. However, more complex aberrations, such as those from keratoconus or a cornea transplant, are not well represented by a Zernike reconstruction of the wavefront.3
Image Selection
Depending on the laser system, an image (or series of images) is selected to calculate the ablation profile; only the highest-quality images should be chosen. The wavefront-derived sphere/cylinder and the manifest sphere/cylinder may differ owing to factors such as accurate technique, accommodation during capture, or the influence of HOAs on manifest refraction.1 It is important to determine the acceptable differences between components of the manifest, cycloplegic, and wavefront refractions to assess acceptability of wavefront data before proceeding with surgery. Some patients may not be ideal candidates for WFG treatment if the deviation is greater than the guidelines recommended by the manufacturer.
Manifest Refraction
Even though the wavefront provides the treatment profile, including sphere and cylinder, a manifest refraction is still necessary. It is primarily used to assess the accuracy of the wavefront capture and to help determine refractive stability. This refraction should be ‘push plus’ to eliminate accommodation, as well as a careful determination of the astigmatism, typically using a Jackson Cross Cylinder. It is important to know the exact refractive status of each patient to properly assess the wavefront data. It is also important to assess and record visual acuity and determine pre- and postoperative visual capability. In this regard, it is useful to assess the full visual potential and not stop unnecessarily when 20/20 is achieved.
Topography
Ectasia is a potentially devastating complication after LASIK and all means are needed to avoid this complication. Our understanding of risk factors has significantly increased over recent years and topography remains an essential tool in this regard. Corneal topography is necessary to evaluate the preoperative corneal shape and rule out preclinical or forme fruste keratoconus. Patients with topographic indications of significant focal asymmetric elevations or maps with clearly-identified pellucid or keratoconic shapes should not undergo LASIK surgery.
Pachymetry
Pachymetry is another important tool used to avoid ectasia. A critical component of LASIK, it is even more important in the use of WFG LASIK as it tends to remove more stromal tissue than conventional treatments. An estimated residual stromal bed is needed for surgical planning and is computed by subtracting the anticipated flap thickness and maximum ablation depth from the central pachymetry. The minimal residual bed for LASIK remains controversial, and though 250 microns is now recognized as the minimum, some surgeons prefer to leave a stromal bed higher than this. To account for variations in actual flap thickness, many surgeons are now measuring the stromal bed after the flap has been retracted (see Figure 3). This allows for a much more precise determination of the residual bed.
Pupillometry and Patient Counseling
Pupillometry remains an area of contention as conventional LASIK has not shown a relationship between the diameter of the low light pupil and disturbing postoperative visual symptoms.4,5 Pupillometry is most often performed today because of litigation concerns. WFG LASIK does not appear to increase symptoms in patients with larger pupils and may have fewer symptoms. In fact, WFG LASIK may provide advantages over conventional LASIK in low light conditions with dilated pupils.1 That is where a reduction, or less induction, of HOAs may be most apparent, which may be of benefit to patients with HOAs. Although custom LASIK has shown fewer postoperative complaints irrespective of pupil size, it is important to counsel patients about the risk for potential postoperative night vision problems.
The WFG LASIK procedure is essentially the same as conventional surgery. The patient is prepped for the procedure and a microkeratome is used to create a corneal flap. An excimer laser is then applied to remove a precise amount of stromal tissue and the flap is repositioned (see Figure 4).
Operative Considerations
Some additional considerations for a custom procedure include:
Alignment and Registration
The alignment of the eye when measured by the aberrometer must match the alignment when the surgery is performed. Similar to astigmatism, most HOAs require torsional alignment. Torsional misalignment during surgery can result in undercorrection of the aberration, or even the induction of aberrations. Hence, proper alignment is a critical component of the surgically correction of HOAs. It has been shown that eyes can undergo up to 13.5° of cyclo-rotation when a patient goes from a seated position measured on the aberrometer to lying under the excimer laser.6 Even small amounts of misalignment can result in a significant undercorrection of astigmatism and HOAs.
Several systems have been developed to ensure alignment. One technique is to mark the limbus, typically at the three and nine o’clock positions, while the patient is seated immediately prior to surgery. These marks are then used to manually align the wavefront image (see Figure 5). More recently, iris registration has been used to automate the alignment process by capturing unique iris details, which are recorded by the aberrometer and relayed to the laser (see Figure 6). Scleral registration is another technique under development to ensure proper cyclo-alignment. This system recognizes unique limbal vessels at both the aberrometer and laser and automatically compensates for misalignment.
Centration
Proper centration of an ablation is critical to ensure good outcomes. Decentration of 0.5 mm or less can result in debilitating visual symptoms.7 Accurate centration is even more important when treating HOAs.8 Centration is based on matching the aberrometer-derived ablation profile to either the limbus or pupil margin. The center of the pupil (pupil centroid) can change positions by up to 0.7 mm as the pupil dilates or constricts.9 For pupil margin-based laser systems, it is important to compensate for this centroid shift to avoid an ablation decentration (see Figure 7). Iris recognition systems do this by using the limbus as a reference point.
Eye Tracking
Even with proper initial centration and alignment, eye movement during surgery can have a deleterious effect on the outcome. Sophisticated eye trackers are employed by all custom-capable excimer laser systems.10 Most systems utilize an infrared camera to track the edge of the iris because of the contrast between the iris and pupil. A passive eye tracker monitors eye motion and interrupts the laser treatment if the eye movement exceeds a certain threshold. An active eye tracker drives a complex mirror system that directs the excimer laser beam onto the proper location on the cornea. Laser systems can employ both methods, steering the laser if eye movements are slight but pausing the laser if movements are too great. This is important because active eye trackers do not account for the change in effective laser energy as the curvature of the cornea changes during movement. Hence, despite having a fully functional eye tracker, the surgeon needs to continually monitor centration during the procedure.
Nomogram Adjustment
Surgical technique, local conditions such as the temperature and humidity, as well as patient characteristics such as gender and age are all potential sources of variability in custom LASIK outcomes. Just as nomogram adjustments are often needed to fine-tune the efficacy of conventional LASIK, so too is it likely that adjustments will be needed to improve the efficacy of a custom treatment.
Femtosecond Flap Creation
Traditionally, LASIK surgery has been performed with a microkeratome. A microkeratome is a precise, hand-held, oscillating blade that is used to separate the layers of the cornea and create a hinged flap that can be lifted back while the cornea is sculpted. Scientific advances have resulted in microkeratomes that are more precise, producing less variability in flap thickness.11
Recent scientific advances have developed a femtosecond laser, which uses infrared laser energy to insert a precise computerized pattern of overlapping spots. The pulse duration is so short that the material is ionized without apparent thermal damage. Thousands of precisely directed spots can create a hinged LASIK flap.12 Both microkeratomes and femtosecond lasers currently utilize a suction ring to hold the eye during corneal applanation (see Figure 8).
There is a growing appreciation that the quality of the flap is even more important when performing custom LASIK. Besides avoiding surgical complications, such as an incomplete or buttonhole flap, the flap needs to be large enough for the custom ablation and to be well centered. Improved outcomes in terms of vision, induced astigmatism, induced HOAs, and enhancement rates are seen to favor the predictability of femtosecond technologies over the microkeratome.13 Despite the added cost, there is a growing body of evidence that shows that the laser flap results in an improved outcome and better quality of vision.14 Femtosecond lasers are able to predictably create flap diameters, hinge location, and flap thickness, while eliminating the risk for cap perforations.15 The technique of flap elevation affects rapidity of visual recovery.
Recent biomechanical studies make a case for thinner flaps (+/-100 microm) that take advantage of the inherent strength of the stromal layers of the cornea, as well as preserving as much corneal tissue as possible. New biomechanical studies comparing corneal response to various types of laser refractive procedures demonstrate that corneal flaps created with a femtosecond laser are the thinnest and most stable.16
Potential difficulties with an ‘all laser’ custom LASIK could arise with tracking failure. In certain cases, very darkly pigmented irises reduce retinal reflection, and, when this is combined with forward light scatter induced by irregular stromal beds, certain laser tracking systems can fail. Delaying the surgery by a few days is usually sufficient to achieve successful tracking.17
Another potential complication may result from the pulse energy used for flap creation with the femtosecond laser keratome. Although there is no loss of uncorrected visual acuity (UCVA), unusual symptoms of photo sensitivity can occur and may be prolonged without prompt steroid treatment. However, this tendency appears to be reduced as new technology uses less pulse energy during flap creation.18
Positive Results of Wavefront-guided Ablation
Highly Aberrated Eyes
A custom re-treatment in patients who have visually disturbing symptoms from previous surgery remains a most intriguing application of wavefront technology. There is great potential to measure and treat aberrations that were induced by previous surgery. Research indicates that custom LASIK following conventional LASIK can successfully reduce HOAs and improve visual quality as shown in Figure 2.19 Because of the ablation depth and healing responses, there can be less accuracy in predicting the postoperative sphere. A hyperopic shift is commonly observed, which can be partially compensated by using a physician offset in the treatment.19 The ability of the wavefront device to accurately capture and measure highly aberrated eyes is important. Overlapping, dropped, or interpolated points in Hartmann-Shack aberrometers is a concern and there must be sufficient resolution and accuracy of the wavefront capture to provide a pattern for treatment. In addition, there must be enough remaining stroma for the procedure. Often, the ablation depth in highly aberrated eyes is much more than anticipated.
Surface Abation
There is renewed interest in applying wavefront technology to surface ablation. The epithelium can either be removed (photorefractive keratectomy [PRK]) or treated as a LASIK flap and repositioned after the ablation (LASEK or epi-LASIK). Anecdotal reports have indicated a better quality of vision with surface ablation compared with LASIK. This may be due to the aberrations induced by the LASIK flap. Panagopoulou and Pallikaris compared the results of WFG PRK and LASIK surgery to conventional.20 Both WFG PRK and LASIK demonstrated improved clinical outcome over conventional treatment. However, the increase in HOAs after WFG PRK (1.3-fold increase) was less than WFG LASIK (1.8-fold increase). The surgical techniques of LASIK and PRK induce distinctly different healing and biomechanical responses. Both of these factors may affect the accuracy of ablations designed to neutralize subtle wavefront errors. In addition, because more tissue generally needs to be removed with a custom procedure, there are patients with insufficient corneal depth to safely perform a WFG treatment. An option in this case is to perform a custom surface ablation procedure. Manufacturers and researchers have clinical trials underway to study WFG surface ablation. Studies that evaluate higher order algorithm adjustments will be complex and are likely to take many years to complete.
Super-normal Vision
Super-normal vision can mean many things. In the context of custom LASIK, it is generally taken to mean the attainment of better vision after surgery than before. The reason for much of the initial excitement regarding wavefront technology was the possibility of obtaining supernormal vision by correcting HOAs.21 Liang and colleagues corrected the aberrations of normal test subjects with an adaptive optical system.22 They reported that through the use of adaptive optics, normal patients can experience significant improvement in high-frequency contrast sensitivity when their HOAs are corrected. In many instances, this goal can be achieved after custom LASIK, but not consistently. Current WFG LASIK cannot reliably reduce naturally occurring HOAs in eyes with lower preoperative amounts. This may be due to a variety of factors, such as subtle mis-alignment of the ablation profile or an unpredictable biomechanical or healing response.
A better understanding of naturally occurring super-normal vision (UCVA better than 20/12.5) could give important insights into the development of WFG refractive surgery. The ultimate goal is to obtain super-vision in normal-vision eyes by correcting not only sphero-cylindrical error, but also HOAs.
While the majority of wavefront error associated with eyes with supernormal visual acuity is sphero-cylindrical, complex aberration patterns are also seen. Most aberrations are formed by a limited number of terms. The largest difference between normal eyes (UCVA 20/25 to 20/16) and supernormal eyes (UCVA 20/12.5 or better) is the amount and type of cylinder. Higher order patterns are very similar between the two populations. There are several Zernike terms and combinations of Zernike terms that seem to be common among all eyes. The overall level of aberrations is much higher than would be expected of a nearly diffraction-limited visual system (more than twice the Rayleigh Quarter-Wave limit). This suggests that excellent vision has a psychophysical component and that image processing may play an important role in super-normal vision.
Conclusion
Custom LASIK is a corneal refractive procedure that requires more attention to detail than conventional LASIK. In addition to standard preoperative exams and measurements, high-quality wavefront images over the entire low light entrance pupil and consistency between manifest refractions and wavefront refraction are important. Similar to conventional LASIK, proper caution must be observed with regard to corneal topography, pachymetry, and other measures of ocular health before surgery.
Where there is greater scientific precision, there exists the possibility of greater results. Incorporating advances in wavefront analysis, flap creation, eye tracking, wavefront registration, and accurate centration, wavefront LASIK offers significant improvements in objective and subjective visual outcomes. It has revitalized corneal refractive surgery with unprecedented success. Although still elusive, the concept of attaining super-normal vision is an intriguing possibility with WFG LASIK and one that is under active investigation.