Premium Intraocular Lenses in Patients who have had Previous Laser Vision Correction
In most of our refractive cataract practices, the people most likely to request premium intraocular lenses (IOLs) at the time of cataract surgery, are those who have had previous kerato-refractive surgery. They may have had surgery many years earlier and enjoyed the benefits of visual freedom and independence, and simply do not want to entertain the idea of having to wear glasses again following their cataract surgery. However, this is the very group where we are generally most nervous of using presbyopia-correcting IOLs (PC-IOLs), as anecdotally, there is evidence that premium IOLs do not work well for these patients.
I was invited to talk at the Refractive Subspecialty Day at the American Academy of Ophthalmology (AAO) Meeting in 2019 on ‘Expanding eligibility for premium IOLs in patients with previous laser vision correction’. As I had only personal experience in using the pinhole optic IC-8 IOL (AcuFocus™, Irvine, CA USA) in these previously treated eyes, I felt I owed the audience a better insight than only my personal experience with the IC-8. I therefore sent out a Survey Monkey poll to almost 150 colleagues; almost 70% of which, replied within the time frame that I had set. I felt confident that I had a truly representative opinion from the most experienced refractive cataract surgeons globally. This article shares my learnings from our colleagues worldwide.
I asked 10 multiple choice questions and some allowed respondents to make comments in certain instances too.
Q1. Do you use PC-IOLs in eyes that have previously undergone kerato-refractive procedures?
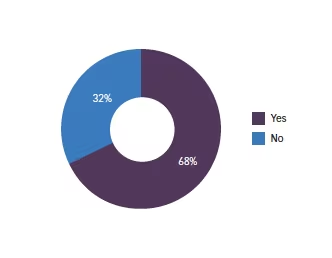
Q2. If your answer to question 1 was no, why is this the case?
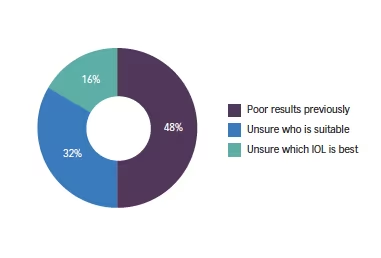
Additional comments that came up frequently were that if the corneal higher order aberrations were low, premium IOLs were more likely to be used with good results. One comment stated that the surgeon was not confident of using multifocal IOLs in first-time procedures with no previous history of corneal surgery, let alone previously treated eyes.
Q3. If your answer to question 1 was yes, are you satisfied with the results so far?
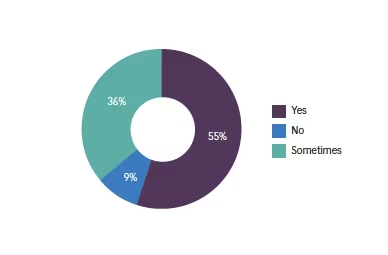
Of these respondents that answered ‘Sometimes’, 47% were happy >75% of the time, and 41% were happy 50–75% of the time; therefore, a total of 88% had a predominantly positive experience in the ‘Sometimes’ group.
Q4. What are the key preoperative criteria to provide a satisfactory result?
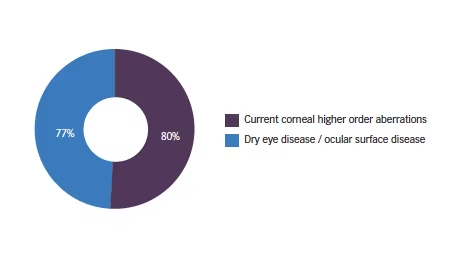
The only other issues that featured heavily were related to patient personality:
- Personality and patient expectations are most important
- If the patient was happy with their previous procedure, they are more likely to be happy with this procedure. The converse is also true.
Q5. Has previous myopia or hyperopia lead to better outcomes?
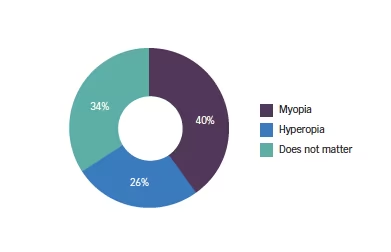
Q6. Does the previous level of hyperopia effect your decision to use a PC-IOL?
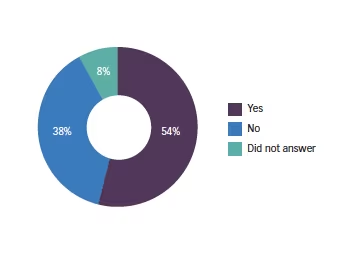
What is the cut-off level where you decide against using a PC-IOL? This varied from +2.00 (a minority) to +7.00 (just one respondent). The majority were between +2.00 and +5.00 as the maximum with the mean value being +3.64D
Q7. Does the previous level of myopia effect your decision to use a PC-IOL?
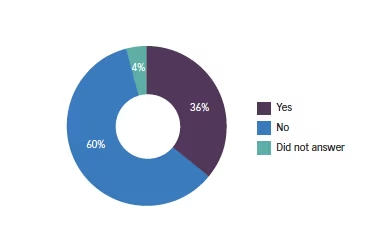
What is the cut-off level where you decide against using a PC-IOL? This varied from -2.00 (a minority) to -8.00 or higher. The majority were between -5.00 and -7.00 as the maximum with the mean value being -6.14D
Q8. What amount of angle kappa is your upper limit?
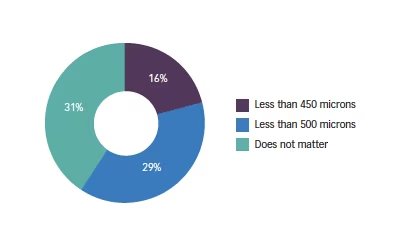
There was a significant variation among the respondents: 16% said <450 microns and 29% said <500 microns. The biggest group (31%) said it did not matter. Some suggested that they never check this parameter and many comments intimated that they did not think it mattered.
Q9. Which PC-IOL design has provided the most satisfactory results in eyes that have previously undergone kerato-refractive procedures?
In order or preference, from best outcomes (1) to poorest outcomes (4):
- AcuFocus IC-8: 1.94
- Trifocal: 2.79
- Multifocal/bifocal: 2.85
- Extended depth of field: 3.14
Q10. What is the most important lesson you would like to share regarding PC-IOLs in previously-treated corneas?
-
- ‘Patient motivation is the strongest driver for surgery. Wrong personality is the strongest negative driver’
- ‘A real cataract, significant current refractive error, stable refractive error, adaptive personality that was happy with the previous LASIK result’
- ‘Patient’s personality needs to be suitable’
- ‘Corneal optics need to be good’
In summary, the following points can be made:
-
-
-
- Up until relatively recently, using a PC-IOL was mostly contra-indicated in eyes that had undergone previous kerato-refractive surgery
- That is clearly no longer the case according to this poll of experts
- Corneal optics and ocular surface are key criteria to ensure a good outcome
- Patient personality is very important and needs to be considered
- The pinhole optic IOL may be best but many are getting good results with other PC-IOLs
-
-
After considering what I learned from the survey and applying my own clinical experience, I follow the guidelines below:
-
-
-
- Let the patient initiate the request for the PC-IOL. They must express the wish to be glasses-free by means of PC-IOLs rather than monovision or blended vision
- I would use the IC-8 IOL if the corneal aberrations are >0.40 microns and only use diffractive multifocal IOLs with errors <0.40 microns
- I would only offer this option to patients that were happy with the laser vision correction outcomes
- An angle kappa of >500 microns still makes me uncomfortable but this is anecdotal
- The possibility of requiring further laser vision correction in the form or photorefractive keratectomy or LASIK (laser-assisted in situ keratomileusis) after IOL surgery needs to be accepted given the greater challenges of achieving the refractive target in previous corneal procedures, especially in cases where the pre-refractive surgery procedure data is not available
- My early experience of the Acrysof® Vivity® (Alcon, Geneva, Switzerland) IOL has been extremely positive and this may become an IOL that I use more frequently in these previous LVC cases
-
-
With this approach I believe that the odds of achieving a satisfactory outcome are increased.




