Examination
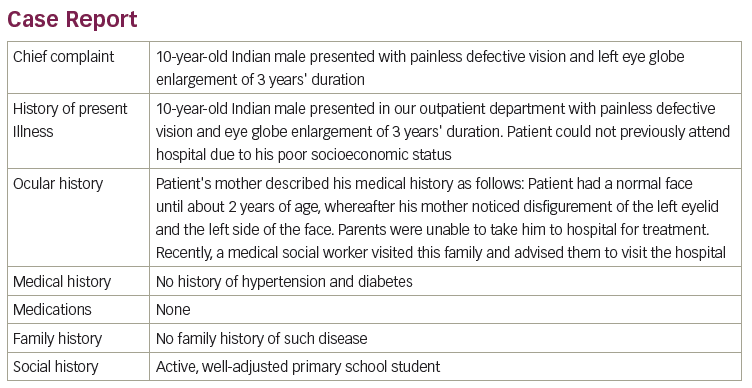
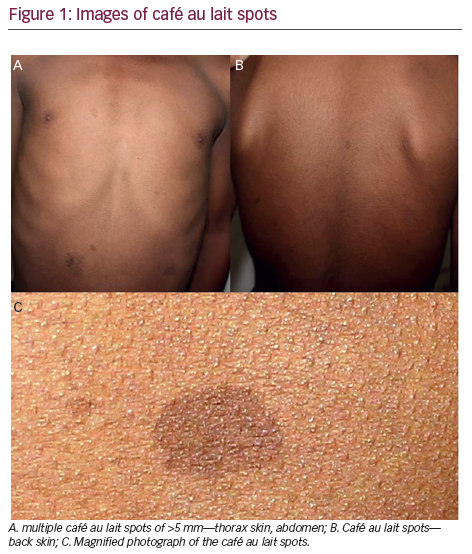
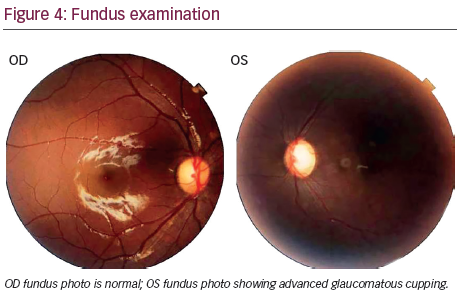
A 10-year-old Indian male with short stature and skeletal deformities presented. Height 120 cm; blood pressure normal. There were multiple café au lait spots of more than 5 mm on the thorax, abdomen, and back skin (see Figure 1). Axillary and inguinal freckling was absent. The left side of the face had hypertrophic deformity due to the plexiform neurofibroma in the maxillary and mandibular region (see Figure 2C). The left upper eyelid had an S-shaped deformity and ptosis (see Figure 2A). On palpation it felt worm-like, consistent with the plexiform neurofibroma. There was marked proptosis and globe enlargement of the left eye (see Figure 2B and 3).The axial lengths of the right and left eye globe were 22.19 mm and 27.99 mm, respectively. The left eye corneal horizontal and vertical diameters were 13 mm each; the right eye corneal horizontal and vertical diameters were 11 mm each. The best corrected visual acuities of the right and left eye were 20/20 and 20/100, respectively. Extra ocular motility was normal. The right and left pupils were 3 mm and 6 mm, respectively. Afferent pupillary defect was noted in the left eye. Intraocular pressure (IOP) in the right eye and left eye were 12 mmHg and 28 mmHg, respectively. The right eye fundus examination was normal. The left eye fundus examination showed advanced glaucomatous cupping (see Figure 4).
Radiologic investigation
A computed tomography (CT) scan and x-ray of the head and orbit were carried out to investigate a possible optic nerve, orbital, or intracranial involvement.
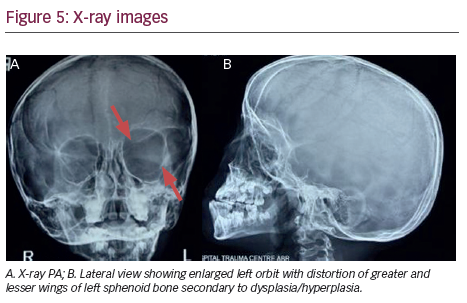
A skull PA x-ray and lateral view showed an enlarged left orbit with distortion of greater and lesser wings of left sphenoid bone secondary to dysplasia/hyperplasia. The central bony orbit also showed altered to poorly appreciated bony landmarks, thus giving the appearance of bare orbit (bare orbit sign) (see Figure 5).
Computed tomography brain
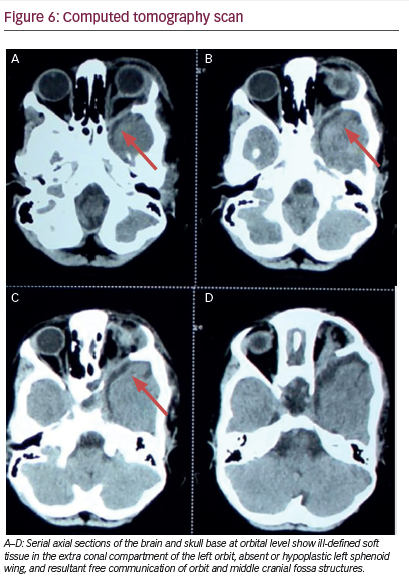
scan A CT brain scan showed absent to hypoplastic greater wing and, to some extent, lesser wing of left sphenoid bone with resultant direct communication of soft tissues of orbit with the left temporal fossa (see Figure 6).
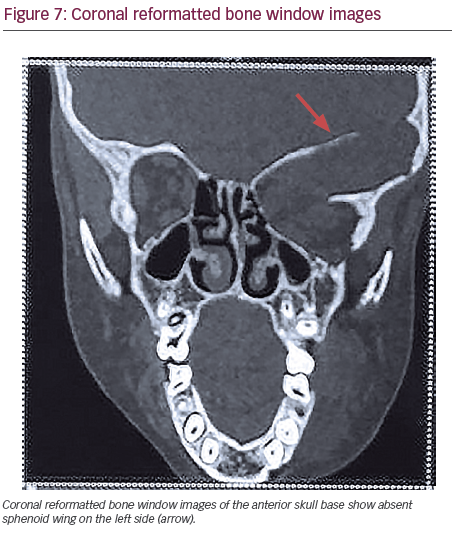
Coronal reformatted bone window images of the anterior skull base showed absent sphenoid wings (see Figure 7).
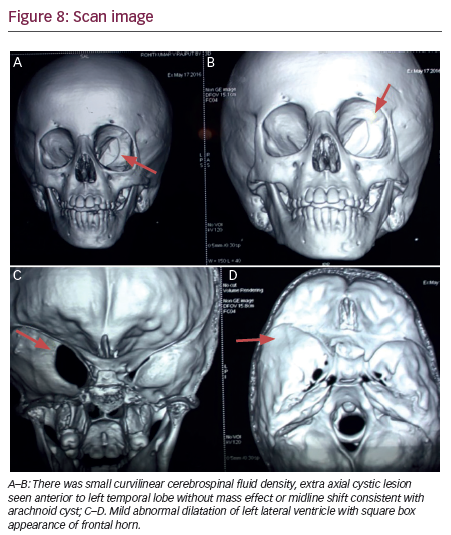
There was mild abnormal dilatation of the left lateral ventricle with square box appearance of frontal horn. The rest of the ventricles appear unremarkable. No obvious periventricular ooze was seen. There was small curvilinear cerebrospinal fluid density, extra axial cystic lesion seen anterior to left temporal lobe without mass effect, or midline shift consistent with arachnoid cyst (see Figure 8).
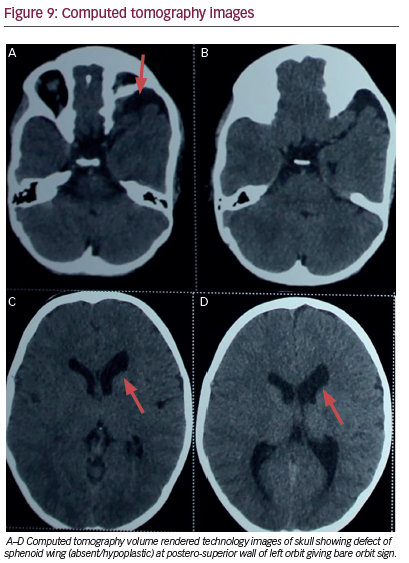
There was gross left proptosis with a relatively enlarged left globe; however, the left globe was normal in shape and attenuation. Ill-defined extra conal soft tissue was noted in the left orbit. Therefore, it was considered that the presence of a neurofibroma was causing proptosis of the left eye globe. Three-dimensional (3D) CT volume rendered technology images of the skull showed an enlarged left orbit with deficient postero-superior wall of the left orbit consistent with absent to hypoplastic sphenoid wing (see Figure 9).
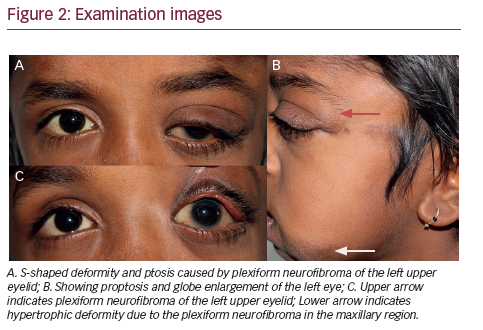
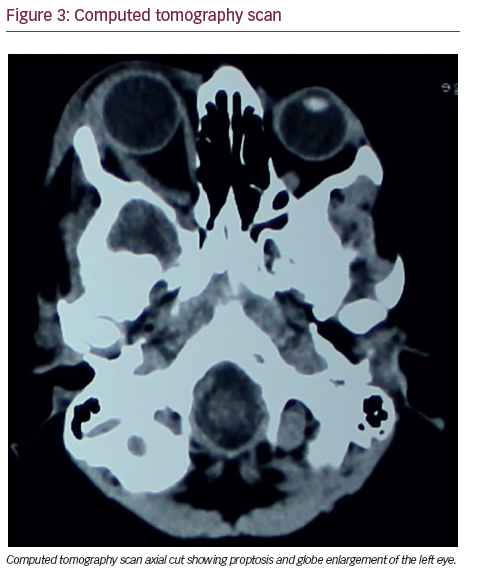
These findings of sphenoid wing dysplasia, dilated lateral ventricle, left exophthalmos, and ill-defined soft tissue in left orbit were consistent with neurofibromatosis (NF) type I.
Management
Left eye trabeculectomy with 0.04% Mitomycin C applications with releasable sutures was performed under general anesthesia. Posttrabeculectomy IOP readings were consistently in the normal range on Day 1, 7, 30, and 90.
Discussion
NF is a rare condition characterized by hamartomas of neural crest origin. The prevalence of NF1 is about one in 3,500 live births.1 The transmission
modality is autosomal dominant; however, approximately 50% of cases are caused by spontaneous mutations, and there is considerable variability of expression between affected families. Diagnosis is usually performed clinically and is based on specific diagnostic criteria. NF is divided into type 1 (NF1 or von Recklinghausen syndrome) and type 2 (NF2, acoustic NF, or central NF).
Eighty-five percent of patients with NF suffer from NF1. The genetic defect in NF1 is almost always a mutation in the neurofibromin gene on chromosome 17 (17q11.2). Neurofibromin normally functions to downregulate the p21 rasoncoprotein. Loss of the neurofibromin tumor suppressor function leads to the proliferation of neural tumors. The most common features of the disease include multiple neural tumors (neurofibromas) on the skin or within the body, pigmented skin lesions (i.e. café au lait spots), and Lisch nodules (pigmented iris hamartomas). Only 10% of NF patients have NF2, which is associated with bilateral acoustic neuromas or schwannomas. The defect in NF2 is on chromosome 22q. In addition to acoustic neuromas, NF2 patients frequently have ependymomas of the spinal cord or multiple meningiomas. Clinical diagnosis of NF1 requires two or more clinical features (see Figure 10).2
Our case had the following clinical features of NF1 criteria: The patient had more than six café au lait spots (>5 mm in diameter) on the thorax, abdomen, and back of the body;2 plexiform neurofibroma of the left eyelid causing S-shaped deformity and ptosis;3 plexiform neurofibroma of the left side of the face caused hemifacial deformity;4 and sphenoidbone dysplasia was seen in x-ray and CT scan.
Although Lisch nodules are common findings in NF1 they were absent in our case. Axillary freckles were also absent.
The right eye was normal. Left eye corneal horizontal and vertical diameters were 13 mm each. The right eye corneal horizontal and vertical diameters were 11 mm each. The axial lengths of the right and left eye globe were 22.19 mm and 27.99 mm, respectively. The left eye had advanced glaucomatous optic atrophy. Morales et al. found that globe enlargement was most severe when associated with glaucoma but also present on the side with orbito–facial involvement in patients without glaucoma. The presence of neurofibroma may induce globe enlargement on the affected side in orbito–facial NF1.3
Glaucoma has been reported in 1/300 NF1 patients.4 Recent studies have made a distinction between NF1 patients with or without orbital– facial involvement—such as plexiform palpebral neurofibroma—and a finding of glaucoma was seen in 23% of the patients with orbital–facial NF1.3 Asymmetric globe enlargement in ipsilateral orbital–facial NF1 was found in patients with glaucoma, with axial lengths ranging from 26 to 36 mm; the difference in the contralateral unaffected eye was

4–6 mm.3,4 In our case, the left eye globe was asymmetrically enlarged; the difference in the contralateral unaffected eye was 5.8 mm.







